These guidelines help people in the hair, beauty and skin penetration industries to comply with the Public Health and Wellbeing Act 2008 (the Act) and the Public Health and Wellbeing Regulations 2009.
Some industry practices are not specifically covered by these guidelines, and new treatments and practices continue to be developed. However, you should still use the general principles of infection control described in these guidelines for these practices.
These guidelines do not replace industry-specific guidelines or codes of practice, which must also comply with the Act and Regulations. You should also talk to the industry association relevant to your business. These guidelines are a guide to best practice and a reference tool for people associated with the industry, including environmental health officers.
The guidelines are divided into five parts:
Part A: Information about registration requirements for premises and relevant legislation.
Part B: General information on how infections are spread and the principles of infection prevention and control that are used to prevent transmission of infection. This includes how to clean, disinfect and sterilise instruments and equipment used to perform personal care and body art procedures.
Part C: Procedure-specific information for:
hairdressing and barbering
facials
cosmetic application (including spray tanning)
eyelash extensions and tinting
hair removal
laser and intense pulsed light
manicure, pedicure and nail treatments
microdermabrasion and dermal-rolling
tattooing (including cosmetic tattooing)
body piercing and other forms of body modification
colonic irrigation.
Part D: Occupational health and safety requirements for hair, beauty and skin penetration industries.
Part E: Glossary
Part F: Appendices
Part A: Registering your premises
Quick guide for business proprietors
The quick guide provides an overview of the main points of registering your business.
The quick guide may not tell you everything you need to know to meet your legal obligations. Use the page references to find out more about each topic.
Registering your business (p. 10)
You must register your place of business (premises) with your local council if you will be doing:
beauty therapy
applying cosmetics
colonic irrigation
hairdressing
skin penetration (piercing)
tattooing.
If you take over a business in existing premises, you need to transfer the registration to your name before you can start trading.
If you plan to start your business in new premises, you should talk to your local council before you choose a site.
Regulations
There are rules you need to follow when you run your business. You must:
keep your business clean and sanitary
use only sterile equipment when you do tattooing or skin penetration procedures
sterilise or safely dispose of any equipment that penetrates skin or has blood on it
make sure you and your staff are clean and have no exposed wounds before doing a procedure
provide easily accessible hand-washing facilities
if you do tattooing or body piercing, keep records of each client, including their name, address and telephone number.
There are age limits for tattooing and body piercing:
You must not do tattooing, scarification, tongue splitting, branding, beading or intimate body piercing on a person under 18 years. Intimate body piercing means piercing genitals, anal region, perineum or nipples.
You must not do non-intimate body piercing on someone under 16 years without the consent of their parent or guardian.
You must not allow a staff member under the age of 16 years to do intimate body piercing.
Your premises
Your premises should be suitable for the procedures you will be doing.
Surfaces that need to be cleaned and/or disinfected need to be made of strong material that you can easily clean and disinfect.
Your premises should have good lighting and ventilation.
Your premises should have separate areas for staff, clients and cleaning/sterilisation.
The cleaning/sterilising area should be big enough for good working practices (see p. 36) Talk to your local council to make sure your premises has everything it needs.
Hand hygiene
You should have a hand washing sink that is used only for washing hands.
You should also use alcohol-based hand rubs, but you still need to have hand-washing sinks. You should provide liquid soap (not bars of soap) for hand washing and disposable paper towels. The sink should be easy to clean, and made of hard, non-scratch material.
The sink should be big enough to stop water from splashing into nearby areas. You should provide a hand-washing sink:
where staff work and where you do procedures
where staff clean equipment and instruments
in or close to toilets.
Equipment cleaning
You should have a sink that is used only for cleaning equipment.
You should not use the equipment cleaning sink for anything else, like making tea or coffee. The sink should have hot and cold running water.
Keeping records
If you are doing tattooing or body piercing, you need to write down the name, address and telephone number of each client.
You also need to include:
the date of the procedure
the type of procedure, including what jewellery was provided and where on the body it was used
the completed consent form
sterilisation records of the equipment you used.
You should keep records at your business for at least 12 months following the date of the procedure.
Animals
You should not allow any animals other than guide dogs or service dogs in the procedure area.
If you do tattooing or skin penetration procedures, it is best not to allow animals in your business at all.
Registration
Under the Public Health and Wellbeing Act 2008 (the Act), if you conduct a business involving:
beauty therapy
application of cosmetics that does not involve skin penetration or tattooing
colonic irrigation
hairdressing
skin penetration (piercing)
tattooing
business that poses a risk to public health (as per the Act)
you must, unless exempt, register the business premises with the local council in which it is located.
If your business involves applying cosmetics (that do not involve skin penetration or tattooing) or hairdressing only, you may conduct a ‘mobile’ business, but you must register your principle place of business.
If you are starting a new business in existing premises, you must:
ensure the premises has current registration with the local council
apply to transfer the registration of the premises to your name before you take over its operation. If you are starting a new business in new premises, before you apply for registration you should:
consult with the local council planning department and environmental health officer to discuss the proposal, preferably before selecting a site
submit detailed plans of the interior layout of the proposed premises to the local council, in accordance with these guidelines
obtain local council approval for the plans before commencing work on the premises
contact Business Victoria for business advice and information
contact the appropriate industry association for industry-specific advice.
Most councils require annual renewal of registrations and conduct annual inspections.
If your business only provides hairdressing and/or temporary make-up services at your premises, you can apply for an ongoing or ‘once-off’ registration. If your business also offers other services (for example body piercing) at the same premises, or you change your services in the future to include other services, you will need the usual annual registration.
If your business is operated by and within the scope of practice of a registered health practitioner under the Health Practitioner Regulation National Law, you may not need to register with the local council.
Registered health practitioners listed in Figure 1 below do not need to register their business. All other registered health practitioners, for example physiotherapist or osteopath, must register their business if undertaking skin penetration procedures.
Figure 1: Exempt health professionals
Dentists
Medical practitioner
Nurses or midwives
Podiatrists
Acupuncturists registered with the Chinese Medicine Board or other registered health practitioner endorsed by their National Board to practice as an acupuncturist
Pharmacists for the purposes of administering vaccines (not for other skin penetration practices, for example, ear piercing)
Business Victoria has information on its website about starting and operating a small business. The Australian Business License and Information Service includes information specific to hair, beauty and skin penetration industries:
Legislation
The Public Health and Wellbeing Regulations 2009 set out the requirements for premises registered under the Act.
You must keep the premises in a clean, sanitary and hygienic condition.
Any piece of equipment or instrument used for penetrating the skin must be sterile at the time of use.
Any piece of equipment or instrument that has penetrated the skin or is contaminated with blood must be either safely disposed of immediately after use or cleaned and sterilised before being used on another person.
Any other used piece of equipment or instrument must be clean before being used on a person.
You must ensure that each person in the business who carries out any procedures on any client keeps themselves clean, and has no exposed cuts, abrasions or wounds, before carrying out a procedure.
You must ensure that easily accessible hand washing facilities are available for use by staff.
You must provide written health information to each client about the potential health risks associated with skin penetration procedures and the information provided must not be misleading.
If you do tattooing or body piercing, you must keep client records, such as name, address and telephone number of each client. Records must be kept for 12 months after the procedure, they must be stored at the premises where the business is conducted, and you must take reasonable steps to protect the information.
The Summary Offences Act 1966 sets out the following requirements designed to protect young people in relation to tattooing, scarification, tongue splitting, branding, beading and body piercing.
A person must not perform tattooing scarification, tongue splitting, branding, beading or intimate body piercing* on people under the age of 18 years.
A body piercer must not perform non-intimate body piercing on someone under the age of 16 years without the consent** of a parent or guardian.
A body piercer must not allow a person under the age of 16 years to perform intimate body piercings*.
* Intimate body piercing includes piercing on the genitalia (including surgically constructed genitalia), anal region, perineum or nipples of a person.
** Consent is considered to be written (including in digital form) consent given in person to the body piercer by a parent or guardian of the person to be pierced; and if the person to be pierced is aged between 10 years and under 16 years the person to be pierced must give their consent also.
Cosmetic injectables
The Drugs, Poisons and Controlled Substances Act 1981 regulates the possession, supply and administration of Schedule 4 (prescription only) drugs. Cosmetic injectable products, such as botulinum toxin type A (Botox® and Dysport®) and dermal fillers (for example, Zyderm®, Zyplast®), are Schedule 4 drugs and, as such, the possession, supply and administration of these drugs must be in accordance with this Act.
Schedule 4 cosmetic injections can only be prescribed by a registered medical practitioner and be administered by a registered medical practitioner or a registered health practitioner (such as a nurse or midwife) under the instruction of a registered medical practitioner.
The extent to which nurses may lawfully possess Schedule 4 drugs is also strictly limited to circumstances described in the Drugs, Poisons and Controlled Substances Regulations 2017.
The Medical Board of Australia also has a guideline for registered medical practitioners who perform cosmetic medical and surgical procedures. The guideline outlines the prescribing and administration requirements for Schedule 4 cosmetic injectables. These include the requirement for a consultation with the patient either in person or by video – not by phone or email.
Australian Standards
Proprietors and staff should be familiar with the Australian Standards as they relate to their premises and businesses. The Department of Health and Human Services (the department) recommends compliance with the standards cited throughout the guidelines as established best practice.
Premises requirements
General requirements
The following general requirements apply to premises registered under the Act.
All equipment, furniture, fittings, floors, walls and ceilings should be constructed of materials suitable for the procedures to be undertaken in the area.
Surfaces that require regular cleaning and/or disinfection should be constructed of a durable, sealed and non-porous material that can be effectively cleaned and disinfected.
There should be adequate lighting and ventilation throughout the premises.
The premises should be designed to provide separate function-specific client, staff and cleaning/sterilising areas.
The cleaning/sterilising area should be designed to ensure movement of instruments/equipment in a one- way direction from dirty to clean to sterile areas
p. 37). It should have sufficient bench space for good working practices and must have separate hand- washing facilities in addition to equipment cleaning sinks.
Plumbing must conform with Victorian Building Authority requirements and Standards Australia. These include:
‘AS/NZS 3500.1:2015 Water Services’
‘AS/NZS 3500.2:2015 Sanitary and Drainage’
‘AS/NZS 3500.4:2015 Heated Water Services’
Premises should have an adequate supply of potable water for all activities conducted at the premises that require the use of water. If this is not possible, you must demonstrate that the use of non-potable water will not adversely affect infection prevention and control of the business.
Premises should be able to effectively dispose of all waste water. For premises not connected to centralised sewerage systems, disposal of waste water must occur into an approved on-site waste water treatment system.
You must talk to your local council planning departments and environmental health officer for specific advice relating to your premises.
Hand-washing facilities
You must ensure that easily accessible hand-washing facilities are available for use by staff. Hand-washing facilities should be:
clearly designated for the sole purpose of washing hands
supplied with liquid soap and single-use paper towel (bars of soap should not be used)
permanent fixtures
hands-free where tattooing and skin penetration procedures are performed (for example, foot, knee or elbow operated or electronically controlled)
made of a hard, durable, non-scratch material and be easy to clean
connected to, or otherwise provided with, a supply of warm running potable water through a single outlet
of a size that allows easy and effective hand washing and will prevent splashing into the adjacent environment.
Hand-washing facilities should be located:
within areas where staff work and where procedures are being undertaken
within areas where staff are cleaning and reprocessing instruments and equipment
within or close to staff and client toilet facilities.
The number and location of hand-washing facilities will depend on the layout and use of areas within the premises. You should talk to your local council environmental health officer to find out where to locate hand-washing facilities.
Portable sinks (i.e. non-permanent fixtures) should only be considered when connecting to the mains plumbing is either very difficult or impracticable, such as for a small make-up kiosk in a shopping centre. You must discuss this option with your local council, and they must approve it before you can install portable sinks.
You should also provide alcohol-based hand rubs in procedure rooms/cubicles for use when hands are not visibly dirty.
Even if you provide alcohol-based hand rubs, you still need appropriately placed hand-washing facilities supplied with liquid soap and paper towels.
Equipment cleaning sinks
Dedicated equipment cleaning sinks with hot and cold running water supplied through a single outlet must be located in the cleaning area for instrument and equipment cleaning.
Equipment cleaning sinks should not be used for purposes other than cleaning reusable instruments and items, for example, tea and coffee making.
Record keeping
If your business does tattooing or body piercing, the Public Health and Wellbeing Regulations 2009 require you to record the name, address and telephone number of each client.
Records must be stored at the premises for 12 months following the date of the last body piercing or tattooing procedure undertaken by the client at the premises.
In addition to the name, address and telephone number of each client, you should also include:
the date of procedure
a description of the procedure(s) and, where applicable, jewellery used and at which site(s)
completed consent form
sterilisation information relevant to the instruments used, such as
sterilisation cycle records, including process-recorder printouts with cycle and chemical indicator pass/fail recorded
records of validation procedures
steriliser servicing records
instrument-tracking records to enable tracing of sets of instruments to individual clients by either manually recording this information on the client record, or having a tracking system that enables this to occur.
Accurate and detailed records are important for both the business and the client if there is any possibility of an infection or blood-borne virus transmission.
Animals
Animals, other than guide or service dogs, should not be permitted in procedure areas.
In general, we do not recommend allowing animals in your premises, particularly if your business undertakes tattooing or skin penetration procedures.
Part B: Principles of infection prevention and control
Quick guide for business proprietors
This quick guide provides an overview of the main points of infection prevention and control. The quick guide may not contain everything you need to know to meet your legal obligations. Use the page references to find out more about each topic.
Preventing and controlling infection (p. 18)
Skin is a natural protection against infection.
However, if skin is damaged, infections can enter the body. Skin can be damaged by cuts or wounds. It is also damaged when it is penetrated by sharp objects, such as in tattooing or body piercing.
If you do hairdressing, beauty therapy, tattooing or skin penetration, you may spread infections. Infections can be blood-borne viruses, like hepatitis B, hepatitis C and HIV.
Infections can also be bacterial or fungal.
Infections can be spread by procedures that do not involve penetrating the skin, such as waxing, manicures and pedicures.
You must understand how to prevent infection so that your business does not spread diseases. You should assume that all blood and body fluids are infectious.
You can use the following precautions to prevent infection.
Hand hygiene (p. 20)
Hand hygiene means washing your hands or using alcohol-based hand rubs. Hand hygiene is the best way to prevent infection.
You should not wear rings, watches or other jewellery when performing procedures, particularly tattooing and body piercing.
If your nails are infected or have a fungal disease, you should not perform procedures until the infection has cleared.
Alcohol-based hand rubs are better than soap and water at reducing bacteria and viruses on your hands. You still need to provide hand-washing basins even if you use alcohol-based hand rubs.
Use liquid soaps. Soap does not need to be antiseptic. You should always wash your hands:
before touching a client
before performing a procedure
after a procedure or exposure to blood or body fluids
after touching a client
after touching something around the client.
You should also wash your hands:
before and after eating
after going to the toilet
before setting up clean/sterile instruments for a procedure
after handling used instruments.
If you use disposable gloves, you should wash your hands before putting them on. You should also wash your hands after you take the gloves off.
Use disposable gloves, plastic aprons, eye protection and face masks (p. 23)
Disposable gloves, plastic aprons, eye protection and face masks are also called personal protective equipment (PPE).
You should use PPE if you could be exposed to blood or body fluids.
Be careful handling sharps (p. 26)
Sharps are anything that can penetrate skin. Types of sharps include:
needles
scalpels
razors
needle bars with needles attached
cannulae (sometimes used for piercing)
glass ampoules
other sharp instruments.
Sharps can be contaminated with blood or body fluids.
You should treat all sharps as contaminated unless you know they are sterile. Always handle sharps carefully to avoid needle-stick injuries.
Always dispose of sharps immediately into a sharps container.
Use an aseptic non-touch technique (p. 27)
An aseptic non-touch technique helps prevent infection during tattooing or skin penetration. To use this technique:
Wash your hands before and after the procedure.
Use gloves and PPE.
Create an aseptic area, and only put sterile items in it.
Clean the client’s skin with antiseptic.
Do not touch sterile items or disinfected skin directly, and make sure they remain uncontaminated — this is why the technique is called ‘non-touch’
If you think an instrument or piece of equipment has been contaminated, replace it immediately.
Be careful handling and dispensing products (p. 29)
Products such as wax, ointments, make-up or creams can easily become contaminated. You should handle these products carefully.
Put a small amount of the product into a separate, clean container. Use only the product from this container on the client.
Use a disposable applicator to apply the product. Only re-dip the applicator into the product you have put in the separate container.
Throw out left-over product. Do not put it back into the original container or use it on another client.
For hot wax and other products that cannot be put into a separate container, use a new disposable applicator each time you dip it into the product.
Linen (p. 29)
Replace linen, paper towels and strips between clients.
Wash linen, towels and protective clothing in hot water (70–80 degrees Celsius). Dry linen on the hottest dryer setting.
Waste management (p. 29)
You need to separate waste into clinical waste and general waste. Use a different bin for each type of waste.
Clinical waste includes:
human blood, body fluid and tissue, and material contaminated with these things
sharps.
You must use a waste contractor authorised by the EPA to remove clinical waste.
Cleaning (p. 31)
Keep your business clean to prevent and control infections. Different types of businesses have different cleaning requirements.
All businesses should have a cleaning schedule for surfaces and equipment.
Reprocessing reusable instruments and equipment (p. 35)
Reprocessing means cleaning, disinfecting and/or sterilising items. Different items have different reprocessing requirements.
You must make sure staff who reprocess items are properly trained. You must have a dedicated area for reprocessing.
Preventing and controlling infection
Skin is a natural defence against infection. However, infections can enter the body if skin is damaged by cuts or wounds, or from penetration by sharp objects, such as tattooing or skin penetration equipment.
When you perform hair, beauty, tattooing or skin penetration services, you can spread blood-borne viruses such as hepatitis B, hepatitis C and HIV.
You can also spread other infections such as bacterial or fungal infections. Unsafe or unhygienic practices can affect the health of your staff and clients.
Even procedures that do not involve skin penetration, such as waxing, manicures and pedicures, can spread infections. These infections include staphylococcal infections such as cellulitis or impetigo, the wart and herpes viruses, and fungal infections such as tinea.
Businesses that provide hair, beauty, tattooing or skin penetration services need to understand about infection prevention and control so that they do not spread diseases.
Source: Staying healthy. Preventing infectious diseases in early childhood education and care services, 5th edition, National Health and Medical Research Council (NHMRC), 2013
Infectious microorganisms (germs), include bacteria, viruses, fungi and parasites. The spread of disease involves the following:
the germ has a source
the germ spreads from the source
the germ infects another person.
All three things must happen for an infection to occur. This is called the ‘chain of infection’ or ‘chain of transmission’.
The source of an infectious microorganism may be an unclean environment or contaminated equipment that has not been appropriately cleaned, disinfected or sterilised between clients.
Infections can also be caused by a person’s own normal bacteria or microorganisms. For example, if equipment pierces the skin, bacteria on the skin can enter the body, allowing them to cause an infection.
There are several ways microorganisms are transferred or spread from their source to infect another person. This can be via droplet, airborne or contact transmission.
The most common way microorganisms are spread in the hair, beauty, tattooing and skin penetration industries is through contact transmission.
There are two types of contact transmission.
direct contact (person to person), when there is physical contact between an infected person and another person
indirect contact, when a carrier or object such as contaminated equipment spreads the infection.
An infection occurs when a person’s body cannot resist an infectious microorganism that enters their body and multiplies. Whether or not the microorganism infects a person depends on the ability of the microorganism to cause disease, and the ability of the person’s the body to resist it. Immunisation is one way to improve a person’s ability to resist certain infections.
Infection prevention and control interventions are designed to break the chain of infection at any of its links.
If any one of the above components is missing, the chain is broken and the potential for infection is eliminated.
Standard precautions
All people potentially harbour infectious microorganisms.
People often do not show signs of disease or infection. They may not know they are carrying an infectious illness such as hepatitis B or C.
Because of this, you must assume that all blood and body fluids/substances are potentially infectious.
Standard precautions means having work practices that achieve a basic level of infection prevention and control. Using standard precautions aims to minimise and, where possible, eliminate the risk of transmission of infection, particularly those caused by blood-borne viruses.
To prevent the spread of infection, you and your staff should always follow standard precautions at all times for all clients.
Clients do not need to tell you if they have a blood-borne virus – you should treat all clients as if they are potentially infectious.
Standard precautions include:
hand hygiene
the use of personal protective equipment (PPE)
the safe use and disposal of sharps
aseptic ‘non-touch’ technique
appropriate handling and dispensing of products
appropriate handling of linen
waste management
routine environmental cleaning
reprocessing of reusable instruments and equipment.
Hand hygiene
Hand hygiene is a general term that refers to any action of hand cleansing, and includes:
applying an alcohol-based hand rub to the surface of hands
washing hands with soap and water.
Hand hygiene is considered one of the most important and effective ways to reduce the spread of infection.
Microorganisms are either present on hands most of the time (resident flora) or acquired during contact with clients, contaminated equipment or environment (transient flora).
The aim of hand hygiene is to reduce the number of microorganisms on your hands, particularly transient flora that may present the greatest risk for infection transmission.
Hand hygiene, when performed correctly, reduces the number of microorganisms on your hands.
Generally, you should remove finger and wrist jewellery such as rings and watches when you perform procedures, particularly skin penetration procedures. This helps to maintain clean hands and decreases the risk of your hands harbouring infectious microorganisms.
We know that artificial nails can spread infections in healthcare settings like hospital. The use of artificial nails in tattooing and skin penetration industries should be avoided as they may interfere with hand hygiene. We recommend that you keep your nails neat, short and clean. Nail polish should be not be chipped.
If you or your staff have an infection of the nail bed or cuticle (called paronychia), or other nail disease such as a fungal infection, they must not perform procedures until the infection has cleared.
What product should you use?
Use an alcohol-based hand rub when hands are visibly clean.
Wash hands with soap and water when hands are visibly dirty and after using the toilet. Alcohol-based hand rubs:
require less time than hand washing
are more effective than washing hands with soap and water when not visibly soiled
are more accessible
are self-drying
cause less skin irritation and dryness than frequent washing with soap and water.
Alcohol-based hand rubs perform better than soap and water at reducing bacterial counts on hands. They have excellent antimicrobial activity against most bacteria and good antimicrobial activity against a range of viruses (for example, hepatitis B or C).
We encourage you to use alcohol-based hand rubs in preference to hand washing in most situations. However, easily accessible hand-washing facilities (hand basin with liquid soap and disposable papers towels) are also essential and must be provided.
The use of other waterless non-alcohol hand hygiene products is not recommended.
Soaps
Plain soaps remove microorganisms by mechanical action and have no antimicrobial activity. They are sufficient for an ordinary hygienic hand wash and for cleansing visibly dirty hands.
You do not need to use antimicrobial soaps (for example, soaps containing chlorhexidine or iodine) in the hair, beauty, tattooing and skin penetration industries. Plain liquid soap is sufficient.
Bar soaps are not recommended as they can become contaminated and spread germs between those using the soap. Liquid soaps are preferred.
We recommend using wall-mounted liquid soap dispensers with single-use liquid soap cartridges/bottles, as these are not able to be topped-up. Free-standing dispensers are also suitable.
If you use refillable soap dispensers, you must wash and dry them before refilling. Do not top them up before they are completely empty.
Alcohol-based hand rubs
When choosing an alcohol-based hand rub, you should consider things like fragrance, colour, texture, skin tolerance and ease of use to make sure your staff will be happy to use the product.
Alcohol solutions containing 70–90 per cent alcohol are the most effective. You should also check to make sure the product has Therapeutic Goods Administration (TGA) approval as a hand hygiene product.
Alcohol-based hand rubs must only be applied to dry hands.
Do not top up alcohol-based hand rub dispensers. Discard the container when empty.
When to perform hand hygiene
Hands can become contaminated with infectious microorganisms through contact with clients, equipment and the environment. Cross-contamination can occur from one site to another on the same client; from client to staff; from staff to client; and from the environment to staff and client.
To reduce the risk of cross-contamination, practice hand hygiene before all contact with clients, and after any activity or contact that could result in hands becoming contaminated.
The World Health Organization’s ‘5 moments of hand hygiene’ can also be applied in the hair, beauty, tattooing and skin penetration industries.
The ‘5 moments’ are:
before touching a client
before performing a procedure
after a procedure or exposure to body fluids/substances
after touching a client
after touching the environment around the client.
There are other times you should practice hand hygiene. These include, but are not limited to:
before and after eating
after going to the toilet
before setting up clean/sterile instruments to use for a procedure
after handling used instruments and equipment.
Using gloves is not an alternative to performing hand hygiene. You should practice hand hygiene before putting on gloves and immediately after taking them off.
Use only single-use gloves. Do not use alcohol-based hand rub on gloves to decontaminate them. Do not wash gloves with soap and water and continue to use them. Take off gloves immediately after a procedure and use appropriate hand hygiene.
If a person performing a procedure needs to leave the procedure area, they must first perform hand hygiene (removing and disposing gloves first) when they leave the area and again when they return to resume the procedure.
How to perform hand hygiene
Refer to the WHO hand hygiene posters for further details of how to wash hands or to use alcohol-based hand rubs.
Method for using alcohol-based hand rub
Remove hand and wrist jewellery.
Dispense the recommended amount of alcohol-based hand rub to the palm of one hand.
Rub the alcohol-based hand rub over all surfaces of the hands including palms, fingertips, back of hands, thumbs, wrists and between fingers until dry, approximately 20–30 seconds. Do not use a towel to wipe hands.
Method for washing hands
Remove hand and wrist jewellery.
Wet hands.
Apply liquid soap and rub over all surfaces of hands.
Wash hands thoroughly, including palms, fingertips, back of hands, thumbs, wrists and between fingers for a minimum of 20 seconds.
Rinse hands well with running water.
Pat hands dry with a single-use towel.
Do not turn off taps directly with hands as this may re-contaminate them. If tap handles are not hands free, use paper towel to turn them off.
Hand care
Skin that is intact (that is, has no cuts, scratches, abrasions, cracks or dryness) provides a barrier against microorganisms. Damaged skin can lead to infection in the person. It may also harbour more microorganisms than intact skin, which increases the risk of transmission of infection to others. As such, hand care is an important component to prevent the transmission of infection.
Frequent hand hygiene can cause some people’s skin to become damaged (known as dermatitis). This may allow microorganisms to enter the body. Frequent and repeated use of hand hygiene products such as soaps, detergents and paper towels can cause the skin to dry out.
Factors that may contribute to dermatitis include:
using products containing fragrances and preservatives – do not use this type of product, or only use small amounts
not wetting hands before applying soap
washing hands with soap and water immediately before or after using an alcohol-based hand rub
putting gloves on while hands are still wet
using hot water for hand washing
allowing skin to dry out
using rough paper towels.
Broken or non-intact skin
If you have a small area of broken or non-intact skin (a cut or abrasion) on exposed parts of your body, you should cover this with a waterproof dressing.
If the cut or abrasion is on your hands, then you should wear single-use gloves during all procedures.
Use of hand creams and lotions
Use water-based hand creams and lotions regularly during the day to help prevent chapped and cracked skin.
Personal protective equipment (PPE)
Assessment of risk
You should provide personal protective equipment for all staff who may be at risk of exposure to blood or body fluids at work.
The type of PPE you choose should be based on a risk assessment of transmission of infection between staff and client, and vice versa.
Source: Public Health England (PHE) 2013, Tattooing and body piercing guideline toolkit.
Clothing
Clothing should not get in the way of maintaining good hand hygiene, for example, wearing sleeves that fall over your hands.
Personal protective equipment protects the clothing and skin from contamination with blood or body fluids/substances.
Do not wear watches or wrist and finger jewellery when working with clients because these items make it harder to maintain hand hygiene and can tear gloves.
Footwear
Enclosed footwear should be worn to protect against injury if sharps or contaminated materials are accidentally dropped.
Check if there are other industry footwear requirements, for example, rubber soled shoes if using electrical equipment.
Gloves
Single-use gloves should be supplied for staff to wear for procedures if there is a potential risk of blood or body fluid exposure. Gloves should be made available in a range of sizes for use by different staff.
Wearing gloves does not replace the need for performing hand hygiene. Gloves may have defects that are not immediately obvious, or they may become damaged during use.
Single-use gloves should be carefully removed to avoid contamination of hands or other surfaces. They must not be washed or reused.
When wearing gloves, gloves need to be changed and/or discarded:
after each client
in between procedures on the same client
if damaged during a task or procedure
on completion of a task or procedure
before handling the telephone or other equipment not related to a procedure.
Gloves are available in a range of different materials, the most common being latex (natural rubber latex). Latex gloves may be the preferred choice because of their tactile sensitivity, barrier property against viruses, good fit and optimal elasticity.
However, some staff and clients may have an allergy or sensitivity to latex. You should provide alternatives to latex, such as neoprene (green coloured) or nitrile (blue coloured) for these people.
Be aware that using petroleum-based lubricants (for example, Vaseline® jelly) alongside latex gloves may affect the glove’s integrity and its ability to protect the person using them.
Always ensure hands are completely dry before putting on gloves. When gloves are worn with other PPE, they are put on last and removed first.
Gloves used for cleaning
Use general-purpose utility gloves (for example, kitchen gloves) for environmental cleaning purposes. Use heavy duty, puncture-resistant gloves for instrument cleaning.
These types of gloves can be reused.
Wash gloves with general-purpose detergent and warm water (or according to manufacturer’s instructions) and stored dry between uses.
Change them when they are damaged or show signs of deterioration.
Masks
Staff should wear masks if blood or other body fluids/substances may splash or splatter into the mouth and nose.
The type of mask best suited to a particular situation depends on the nature of the activity. There are two main types of mask used in skin penetration procedures and cleaning.
Surgical-style face masks reduce the risk to staff from splashing and spraying of body fluids/substances. They are generally loose fitting without a tight air seal, and they are not efficient in preventing the wearer from inhaling airborne particles. They should be fluid resistant. See ‘AS/NZS 4381:2015 Single-use face masks for use in healthcare’.
Particulate filter personal respiratory protection devices (P2 respirators) are close fitting and capable of filtering up to 95 per cent of airborne particles. They may also be referred to as an N95 respirator or mask. See ‘AS/NZS 1715:2009 Selection, use and maintenance of respiratory protective devices’, and ‘AS/NZS 1716:2012 Respiratory protective devices’.
When using lasers, you may need to wear a mask to reduce the risk of inhaling of airborne contamination in accordance with ‘AS/NZS 4173:2018 Safe use of lasers and intense light sources in healthcare’.
Check the manufacturer’s recommendations. Masks should:
be fitted and worn according to the manufacturer’s instructions
not be touched by hands while being worn
cover both mouth and nose while being worn
be changed between clients
be removed by touching the ties and loops only
not be worn loosely around the neck; must be removed and discarded immediately after use.
Eye protection
Staff should wear eye protection if there is a risk of blood or body fluids/substances splashing into the eyes. This is particularly relevant during cleaning procedures, although good cleaning practices should keep the risk of these events to a minimum.
Various types of eye protection are available, including goggles, face masks, visors and full-face shields, which have either reusable or single-use guards. If you use reusable goggles/shields, wash them after each client or task using a general-purpose detergent, rinsed and stored dry.
‘AS/NZS 4173:2018 Safe use of lasers and intense light sources in healthcare’ specifies that eye protection specifically designed for the wavelength and classification of the laser in use must be worn by all within the laser-controlled area. Check the manufacturer’s recommendation for the required type of eyewear.
Aprons/gowns
Wear waterproof aprons or gowns when there is a risk of clothing being contaminated with blood or body fluids, and also when undertaking cleaning procedures.
Use single-use aprons and change the apron between clients or tasks.
Safe use and disposal of sharps
Sharps are anything that can penetrate the skin.
Sharps can include items such as needles, scalpels, razors, needle bars with needles attached, cannulae (sometimes used for piercing), glass ampoules and other sharp instruments can penetrate the skin.
Sharps may become contaminated with blood or body fluids, or other hazardous substances (for example, medications or chemicals). Unless you are certain they are sterile, you should consider all sharps contaminated.
You should always practice safe handling, use and disposal of sharps. This will help to prevent injury and possible transmission of disease to staff and clients.
Handle all sharps carefully, particularly during procedures, to avoid needle-stick injuries and the possible transmission of blood-borne viruses.
The risk of sharps injuries can be significantly reduced when the person using or generating the sharp takes responsibility for its safe management, and immediately disposes of it after use into an appropriate container.
Sharps are considered clinical waste and must be disposed of into an appropriate sharps container. Suitable sharps containers should be:
clearly labelled
rigid walled
puncture proof
with a tight-fitting lid.
These containers can vary in size. Make sure you use a container that is the appropriate size for the type and volume of sharps you use in your business.
Do not overfill sharps containers. Sharps containers can be:
non-reusable, and should comply with ‘AS 4031:1992 Non-reusable containers for the collection of sharp medical items used in healthcare areas’, or
reusable, and should comply with ‘AS/NZS 4261:1994 Reusable containers for the collection of sharp items used in human and animal medical applications’.
Sharps containers should be placed a minimum of 1 metre above floor level, out of the reach of children. They should also be placed in a secure position or mounted on the wall to prevent tipping.
When the container is full, seal and dispose of it in accordance with Environment Protection Authority (EPA) Victoria requirements.
Aseptic non-touch technique
Use an aseptic non-touch technique to prevent contamination during invasive (skin penetration) procedures. This technique aims to prevent infectious microorganisms from being introduced to susceptible sites by hands, surfaces and equipment.
Aseptic non-touch technique can be applied in any setting and needs to be maintained during all procedures.
Aseptic non-touch technique involves:
effective hand hygiene before and after the procedure
appropriate use of gloves and personal protective equipment
creating of an aseptic field/zone on which you only place sterile items
opening and introducing packages/instruments/fluids to the aseptic field/zone in such a way as to avoid contamination
cleansing the client’s skin with an antiseptic
ensuring you do not directly touch sterile items and disinfected skin again to prevent contaminating them (thus using a ‘non-touch’ technique)
ensuring all sterile items and disinfected skin remain uncontaminated
if at any time you think you may have contaminated an instrument/piece of equipment, replace it immediately.
Preparation of the client’s skin
Most infections following skin penetration procedures are caused by the normal flora (microorganisms) of the client’s own skin or mucous membranes.
It is very important to properly prepare the client’s skin before undertaking any skin penetration procedure.
The client’s skin should be visibly clean and free from cuts, abrasions and any visible sign of infection. If the skin is soiled, wash the area with a plain liquid soap and water and dry it before applying any skin antiseptic solutions. Disinfect the area just before to you start the skin penetration procedure.
Apply the antiseptic to the skin using a clean, single-use swab. You must allow the antiseptic to dry completely. Do not wipe off excess solution. Do not touch the area after the antiseptic has been applied (for example, to test for dryness), as this will re-contaminate the skin.
Discard any remaining antiseptic at the end of a skin penetration procedure. Observe the use-by dates on antiseptics.
Which product to use?
An antiseptic is an antimicrobial substance, usually a solution, that can be used on skin or tissue.
Use antiseptics to prepare a client’s skin before a skin penetration procedure to reduce the risk of infection. As such, it is very important to use an appropriate antiseptic product to disinfect the skin before any skin penetration procedure.
Use any one of the following antiseptics to disinfect skin:
70 per cent w/w ethyl alcohol
80 per cent v/v ethyl alcohol
60 per cent v/v isopropyl alcohol
alcohol (60 per cent w/w isopropyl or 70 per cent w/w ethyl) formulations of 0.5 per cent to 4 per cent w/v chlorhexidine
aqueous formulations of 0.5 per cent w/v chlorhexidine
aqueous or alcohol povidone-iodine (1 per cent w/v available iodine).
Ask the client if they have an allergy to alcohol, chlorhexidine or iodine-based products before using any of these products on their skin. Clean areas around the eyes with only warm water or an aqueous (water- based) skin antiseptic; do not use an antiseptic with chlorhexidine near eyes. If you are unsure whether an antiseptic is water-based or not, just use warm water.
Iodine solutions are generally not suitable when tattooing as they may affect the colours of the tattoo.
Use single-use swab packets or sachets of skin antiseptic products instead of large containers intended for multiple use, as these can become contaminated. If you do use a multi-dose container, date the container when opened; discard within 30 days of opening or if not managed in an aseptic manner.
Appropriate handling and dispensing of products
Products that may be used on several clients, for example wax, ointments, make-up or creams, can easily become contaminated if you do not handle them in a way that prevents contamination.
Use the following processes to avoid contaminating multi-use products:
Dispense the amount of product that you will use on the client into a separate, clean container. Use only the dispensed product on the client.
Use a clean (preferably disposable/single-use) applicator to apply the product. Never re-dip the applicator into the original product and/or container – only re-dip into the dispensed product.
Discard any leftover dispensed product. Do not return leftover product to the original container or use it on another client.
If a product cannot be dispensed into a separate container for use (for example hot wax), use a separate, clean (preferably disposable/single-use) applicator each time to dip into the product. Never re-dip a used applicator into the original or multi-use container.
Use products in accordance with the manufacturer’s recommendations. Do not dilute or mix with other chemicals or products unless specified by the manufacturer.
Pumps, spray bottles and nozzles
Pump outlets, bottles and nozzles can be a source of contamination, particularly if contents build up around the outlet. Clean nozzles frequently and dry them before use.
Do not top up refillable liquid soap, pump/spray bottles and other reusable dispensers. This can cause contamination. Always empty bottles before washing them and the nozzles in warm water and detergent, rinse under hot running water, and dry using a lint-free cloth. The bottle can then be refilled.
Drop-in single-use cassette dispensers may be more convenient and economical.
Appropriate handling of linen
You should use paper towel, paper strips and/or sheets or clean linen that is changed between clients. Place soiled linen, towels and protective clothing in a washable, leak-proof container, and wash them in hot water (70–80 degrees Celsius) and detergent. If hot water cannot be used to wash linen, you should add a sanitiser or disinfectant (for example, Napisan®) to each load.
Dry linen on the hottest dryer setting.
Store all clean linen, towels and clothing in a clean environment to prevent contamination.
Waste management
Appropriate and safe waste management is important for the prevention of transmission of infectious diseases. This protects your staff, clients, people who deal with waste downstream, and the community in general.
Management of waste must conform with EPA Victoria requirements, in particular, the management of clinical and related waste.
Waste separation
You need to separate waste into clinical and related waste and general waste at the point of generation. This means having separate bins for different types of waste. Separating waste allows for safe and correct disposal. It can also help with recycling and waste reduction.
You should line all bins with a plastic bag that can be sealed for disposal.
You should make sure that waste is properly separated, packaged, labelled, handled and transported. This will minimise the risk of occupational injuries, such as needle-stick injuries. It will also reduce the chance of exposing waste handlers and the community to infection.
Clinical and related waste
This type of waste is generated in a clinical or similar setting (for example, waste from skin penetration activities or tattooing), and has the potential to cause disease, injury, or public offence.
Types of clinical waste include:
human blood, body fluids and tissue (excludes hair, nails, urine and faeces)
a sharp discarded object or device capable of cutting or penetrating the skin (‘sharps’)
materials or equipment contaminated with, or reasonably suspected of being contaminated with, human blood or body fluids (other than urine or faeces).
Hair, nails and materials or equipment contaminated with urine and faeces may be disposed of in general waste.
Clinical waste also includes items such as blood-stained swabs or cotton wool and gloves.
You should place clinical and related waste in a bin lined with a yellow plastic biohazard bag. The bin should have a close-fitting lid marked ‘clinical waste’. You should wash the bin regularly.
Clinical waste should be disposed of according to EPA Victoria legislative requirements. All clinical and related waste in Victoria should be transported by an authorised EPA Victoria contractor.
General waste
General waste is any waste that does not fall into the clinical and related waste categories, such as papers and powdered pigments. You can further divide general waste into recyclable and non-recyclable materials.
You should place general waste in a bin lined with a plastic bag. The bin should have a close-fitting lid marked ‘general waste’. You should empty the bin regularly, so it does not overflow. You should wash the bin regularly.
General waste can be disposed of via normal refuse collections.
Liquid waste
All liquid waste may be disposed of via the sewer, provided the local water authority has given prior permission. Plumbing should meet relevant regulations and standards
Liquid wastes must not be disposed of into hand basins or equipment cleaning sinks. The risk of contamination of sinks is high, which can lead to contamination of hands or instruments washed in these sinks. It is best if you provide a ‘cleaner’s sink’ or designated ‘dirty’ sink.
Routine cleaning of premises
Transmission of infectious agents from the environment to clients may occur if the client has direct contact with contaminated equipment. It may also occur indirectly, for example, if you touch contaminated equipment or the environment and then touch a client.
Cleaning physically removes organic material such as blood and body fluids, along with dirt and dust. Cleaning does not necessarily destroy microorganisms from the item that is being cleaned. However, providing and maintaining a clean and easily cleanable environment can prevent and control infections. This includes ensuring equipment and work surfaces are suitable for the purpose, can be kept clean (that is, impervious surfaces) and are maintained in good physical repair.
Specific cleaning requirements will vary for each business type. However, all businesses need a written cleaning policy that includes:
routine, scheduled cleaning of all surfaces and equipment to reduce dust and dirt
a cleaning protocol for blood, body fluids and other spills.
A risk assessment will determine the cleaning method, frequency, and products and equipment required.
You should have a cleaning schedule that ensures your business premises is systematically and appropriately cleaned. The table below provides some guidance on frequency and method for cleaning of some items or surfaces.
Cleaning method
Effective cleaning consists of a combination of mechanical action, detergent and water. Most hard surfaces can be adequately cleaned with warm water and detergent. You need to ensure surfaces dry rapidly (or are dried), because moisture encourages microorganism growth.
You can also use a disinfectant solution on surfaces where there is a higher risk of contamination with infectious agents. If you are not using a combined cleaning/disinfectant product, you should use the disinfectant after physical cleaning with water and detergent.
Dry-mop floors first to remove debris before washing floors with a damp mop. Do not use a broom, as sweeping disperses dust and microorganisms into the air.
Clean from the least dirty surfaces or areas (least contaminated) to the dirtiest surfaces or areas (most contaminated). For example, clean a pedicure chair before cleaning the footbath. Cleaning this way will help to prevent spreading germs from the most contaminated and dirty surfaces to areas that have fewer germs.
Cleaning and disinfectant products
Detergents
Single-use disposable detergent wipes are useful for spot cleaning. There are many brands of suitable detergent wipes in varying sizes available. These eliminate the need for preparing daily solutions.
Discard wipes after use.
Disinfectants
Disinfectants can reduce the number of microorganisms on a surface, but they are not a replacement for thorough cleaning. The cleaning process determines the effectiveness of any disinfectant.
You do not always need to use disinfectant, but you may use it on surfaces at high risk of contamination with blood or body fluids. Always clean with detergent and water before using a disinfectant.
Alternatively, you can use a commercially available combined disinfectant/detergent product, as long as you still clean manually. Do not mix any other chemicals or products with detergents or disinfectants, unless specified by the manufacturer.
Detergent or disinfectant solutions should be prepared and used in accordance with the manufacturer’s directions.
You should write the date on the container when you open it and discard the product as per the manufacturer’s recommendation.
Solutions diluted for use should be discarded after 24 hours or as per manufacturer’s instructions. Do not top up detergents or disinfectants as this may lead to contamination.
Discard leftover solutions and wash and dry dispensing bottles/containers before dispensing more product or preparing fresh solutions.
Hard surface disinfectants are regulated by the Therapeutics Goods Administration (TGA). The equivalent of a hospital grade disinfectant should be used in registered premises.
Note:
Hard surface disinfectants must not be used to disinfect instruments or equipment for use on clients.
Use of bleach (sodium hypochlorite)
Bleach is commonly used as an environmental disinfectant. The following points are important to remember when using bleach.
The disinfectant of choice for general disinfection of the environment is usually a hypochlorite solution containing 1,000 parts per million available chlorine (ppm avCl).
To make a dilution of 1,000 ppm avCl from household bleach (with 4 per cent available chlorine), use a 1:40 dilution. Add 1 cup (250 mL) of bleach to 10 litres of water (a standard bucket holds approximately 9–10 litres); or 25 mL to 1 litre of water for a smaller volume.
Mix a fresh solution of diluted bleach, either daily or as required. Hypochlorite solutions are unstable and should be made up daily.
To prevent deterioration, store bulk bleach containers in dark, cool areas (and strictly adhere to use- by dates on bleach products).
Wear PPE (gloves, apron and eye protection) when handling bleach, because it can cause skin irritation.
Leave the bleach solution on the surface you are cleaning for 10 minutes then rinse it off.
Dry the surface.
You do not need to routinely use bleach or other disinfectants for surfaces. Cleaning surfaces with detergent alone is usually sufficient. Use a disinfectant when surfaces are contaminated with blood or body fluids.
Cleaning equipment
Cleaning equipment should be fit for purpose, easy to use and well maintained. Handles on mops should be made of a non-porous material such as aluminium, not wood. You should store cleaning equipment in a designated area after use.
Reusable cleaning cloths need to be washed (laundered) and dried after use. Sponges cannot be cleaned, so unless you discard sponges after each use, you should not use them. Consider using single- use cleaning cloths.
Buckets and mop heads need to be washed then rinsed clean in hot water after use, and the mop heads wrung out and hung to dry (store upside down).
Use squeeze bottles rather than spray bottles for applying cleaning chemicals. Spray bottles can aerosolise chemicals which can be a health hazard for staff and clients.
You should label all bottles used to dispense cleaning chemicals.
Cleaning standards for change/shower rooms and toilets
All surfaces should be free from smudges, smears, body fats and mineral deposits. Surfaces include plumbing fixtures, tiles and other polished surfaces. Sanitary disposal units should be regularly emptied.
Clean-up procedures for blood or body fluids spills
Blood and body fluid spills need to be cleaned promptly to reduce the potential for contact with other clients, staff or visitors. The table below provides guidance for appropriate management of spills of varying size.
Source: NHMRC 2010, Australian guidelines for the prevention and control of infection in healthcare.
You do not need to use bleach (sodium hypochlorite) for routinely managing spills, but you may use it in specific circumstances. You should decide to use sodium hypochlorite based on a risk assessment of the environment (hard surface vs soft furnishings), the spill (type of body fluid and size), risk of transmission of disease (whether the surface is frequently touched by clients and staff) and the potential hazards of using the product.
Reprocessing of reusable instruments and equipment
Reprocessing means cleaning, disinfecting or sterilising instruments and equipment for reuse on another client.
You should always purchase instruments and equipment that can be appropriately reprocessed.
Where possible, you should use pre-sterilised single-use items instead of reprocessing reusable instruments and equipment.
Reprocessing of reusable instruments and equipment can include:
cleaning – removing contamination and foreign material (for example, soil and organic material) from items to the level required either for further processing or reuse of the item
disinfection – a process that inactivates microorganisms (but not bacterial spores) on an item to a level appropriate for reuse of the item
sterilisation – a process used to make an item free from viable microorganisms, including bacterial spores.
The minimum level of reprocessing required for an item is based on the risk it poses to the transmission of infection.
The Spaulding classification is a system used to classify items according to the degree of risk for causing infection based on how the item is used. The system specifies the minimum level of reprocessing that is required.
Table 5 below outlines the Spaulding classifications, the level of reprocessing required and examples of items commonly used in the hair, beauty, tattooing and skin penetration industries.
For further information regarding the level of reprocessing required for commonly used items, refer to the tables ‘Cleaning and reprocessing requirements for equipment used’ in each of the procedure specific sections in
Use the following principles when reprocessing reusable instruments and equipment:
Handle reusable instruments and equipment in a way that prevents staff, clients and the environment from coming into contact with potentially infectious material.
Reprocess all reusable instruments and equipment according to their intended use and manufacturer’s advice.
Before purchasing any reusable instruments or equipment, ensure that you read and are able to follow the manufacturer’s reprocessing instructions.
Do not reprocess any item labelled single-use and/or marked with the symbol, as per Therapeutic Goods Administration (TGA) regulations.
Using single-use items (and discarding them) removes the need to reprocess items.
Clean and sterilise items used in association with skin penetration after use. If this is not possible (for example, tattooing motors), use an impervious cover to minimise the possibility of contamination. Use only single-use covers. After use, carefully remove the cover so it does not contaminate the item and disposed of the cover. The item must then be cleaned and disinfected.
Clean and sterilise reusable instruments and equipment contaminated with blood. If items cannot withstand sterilisation, clean and disinfect them.
If an item cannot be cleaned, it cannot be disinfected or sterilised (and therefore cannot be reused).
Staff training
You must train staff who reprocess instruments and equipment for reuse in:
cleaning of equipment, including using detergents and other reprocessing equipment correctly
the disinfection process
preparing items for sterilisation and correctly using, monitoring and maintaining the steriliser (if applicable)
correct storage of reusable instruments and equipment
detecting problems in the process and taking action to correct issues. You should keep records of all staff training you provide.
Equipment reprocessing area
If your business reprocesses instruments and equipment, you must provide an area dedicated to this task. The reprocessing area can be a separate room or a dedicated part of a treatment area.
Items to be reprocessed must flow along a defined pathway from used/dirty through cleaning, to disinfection or sterilisation, then to clean storage and return to use.
A one-way workflow will ensure that dirty reusable instruments and equipment do not come into contact with clean or sterilised reusable instruments and equipment. Figure 3 below indicates a suggested layout and workflow for an equipment reprocessing area.
Adapted from Royal Australian College of General Practitioners (RACGP) 2014, Infection prevention and control standards for general practices and other office-based and community-based practices, 5th edition, and Alberta Health Services, Infection prevention and control best practice guideline for foot care devices
Bench surfaces in the reprocessing area should be made from an impervious cleanable material, such as stainless steel. If surfaces are chipped or damaged, they cannot be adequately cleaned, and can harbour microorganisms. Keep surfaces clear of clutter to allow adequate cleaning and prevent accumulation of dust.
The size of the reprocessing area and the equipment you need (for example, an ultrasonic cleaner) will depend on the procedures your business performs and the number of instruments that need to be reprocessed.
If you use only disposable equipment, and do not reprocess instruments or equipment in any way, you do not need to have an equipment reprocessing area.
Equipment-cleaning sinks
The equipment processing area should have two sinks: a ‘dirty’ sink for washing and a ‘clean’ sink for rinsing washed reusable instruments and equipment.
Do not use equipment-cleaning sinks for hand washing (and do not use hand basins for cleaning instruments and equipment).
Cleaning reusable instruments and equipment
Clean items before the disinfection or sterilisation process. This ensures proper disinfection and sterilisation.
Clean items as soon as possible after use to prevent soil drying onto the instruments or equipment. If soil dries or hardens on an item, the cleaning process will be more difficult and may be less effective.
If you cannot clean the instrument immediately, cover it in warm water to prevent blood and body fluids from drying. Do not leave instruments soaking for longer than one hour. Leaving instruments to soak for prolonged periods may lead to increased bacterial growth, biofilm formation and damage to instruments (for example, rusting), which makes cleaning less effective. If an instrument cannot be immersed in water, you should clean it immediately.
Instruments that can be disassembled must be disassembled before the cleaning and disinfection or sterilisation process.
Manual cleaning
Generally, manual cleaning (cleaning items by hand) is the best cleaning method in hair, beauty, tattooing and skin penetration businesses.
Use manual cleaning when items need to be carefully handled and are not suited to automated cleaning methods.
You should always wear appropriate PPE while cleaning. This includes a plastic apron, heavy utility gloves and face protection when necessary. You should take care to prevent splashes to the face or injuries with sharp instruments.
Method for manual cleaning:
Pre-rinse items in warm running water to remove soil.
Fill the sink with warm water and detergent to the concentration recommended by the manufacturer.
Dismantle or fully open items to ensure all parts are thoroughly cleaned.
Immerse items (a few at a time) in the sink with warm water and detergent.
Scrub items using a firm-bristle nylon brush. Hold the items low in the sink to prevent scrubbing from creating droplets in the air that you might breathe.
Wash all surfaces of the items, including the inside of tubes and valves.
Rinse items in warm to hot running water in the second ‘clean’ sink.
Dry items in a drying cabinet or with a clean lint-free cloth. Do not allow items to air dry or drip dry.
Visually inspect items for cleanliness.
You should use detergents that are low-foaming, nonabrasive, noncorrosive, biodegradable, free-rinsing, non-toxic, and of a mild alkaline formulation. Do not use common household detergents because they have high-foaming properties and their oily residue is difficult to rinse off.
Do not use abrasive cleaners such as steel wool or gritty powders/pastes as they damage the surface of instruments and leave residues.
Cannulated (hollow or lumened) items such as stainless-steel receiving tubes used in body piercing are a particular challenge to clean. Immersion in an ultrasonic cleaner may assist in the manual cleaning by removing or loosening soils.
Reusable tubing is also a challenge to clean and has the potential to generate infectious aerosols. Use single-use tubing instead.
Non-immersible Items
Items that cannot be fully immersed in water should be wiped with a lint-free cloth dampened in warm water and detergent, then rinsed and dried. Wipe the item over with a 70 per cent ethyl alcohol solution to chemically disinfect.
Automated methods of cleaning
Ultrasonic cleaners
You can use an ultrasonic cleaner for some parts of the cleaning process (depending on the fragility of the item).
Ultrasonic cleaners do not sterilise or disinfect instruments, but they provide a safe and effective means of cleaning most reusable instruments before sterilisation.
Ultrasonic cleaners work by producing high-frequency, high-energy sound waves that cause organic material to dislodge and drop to the bottom of the tank, or to be loosened enough that it can be rinsed off.
Follow the manufacturer’s instructions when using an ultrasonic cleaner.
Washer–disinfectors
Washer–disinfectors are closed cabinets that are plumbed to the water supply and drainage system.
You need to load instruments into a washer–disinfector carefully. Disassemble instruments as much as possible and do not stack items.
Washer–disinfectors need to be regularly cleaned and maintained to prevent contamination of instruments cleaned in the machine.
Cleaning for off-site sterilisation
Instruments being sterilised offsite should be cleaned and packaged before being transported.
Transport loose instruments in a clean, closed puncture-proof container, to ensure they are not damaged in transit.
Some off-site sterilising services may wish to do the packaging. In this case, you still need to clean instruments before transport.
Drying instruments/equipment
Do not dry items in ambient air (for example, on a bench), because this will allow airborne contamination.
Use a clean, lint-free cloth to dry items. Paper towelling is not appropriate because it is not lint free.
Once items are dry, you can handle them with clean, ungloved hands.
Do not handle cleaned items or packaging materials if you have recently used a hand cream/lotion. Wash your hands first. Hand creams/lotions, especially oil-based ones, will leave marks that may attract contaminants and provide an impenetrable barrier to steam.
Make sure equipment wiped over with a 70 per cent alcohol solution is dry before storage.
Disinfection of reusable instruments and equipment
Chemical disinfection has far lower levels of quality assurance than steam sterilisation, and must not be used on critical or high-risk items used to penetrate the skin.
Using disinfectants does not replace good cleaning practices. All items should be thoroughly washed and dried before disinfection.
Disinfectants may be used when equipment is contaminated with blood or other body fluid/substances and cannot be sterilised.
Items that can be sterilised must be cleaned and sterilised before reuse when contaminated with blood or body fluid/substances.
Note:
Disinfectants can easily become contaminated and are a potential source of infection. Solutions should be labelled appropriately (with the name, date and dilution strength).
Do not mix detergent or disinfectant solutions, because they may react with each other and, in doing so, reduce their effectiveness or cause harm. Always follow the manufacturer’s instructions.
Some disinfectants, such as those that are chlorine-producing, should be freshly prepared just prior to use.
Disinfection processes
Thermal disinfection
Thermal disinfection uses heat and water at temperatures that destroy most organisms. It is the most cost-effective and efficient method of disinfection. It is only suitable for items that can be fully immersed in water at high temperatures.
All items should be fully immersed for the entire time once the water boils (see Table 6). Do not add additional items during this boiling stage. If the water temperature cannot be maintained for the time required, this method of disinfection will not be suitable.
Thoroughly clean and dry items before the thermal disinfection process
Thermal disinfection is suitable for items that can be fully immersed but do not need to be sterile at the time of use.
Chemical disinfection
Only use chemical disinfection when thermal disinfection is unsuitable. Consider each chemical and its use carefully and follow the manufacturer’s instructions. Only use a disinfectant for the approved purpose.
The following principles of disinfection apply.
All items should be cleaned and dried before chemical disinfection
You must dry items fully after cleaning and before either wiping or immersing the item in a chemical disinfectant. This is because any moisture/fluid on the item will dilute the chemical disinfectant solution, making it ineffective.
If immersing items in disinfectant, use a container with a close-fitting lid. Fully immerse items for the time specified by the item/equipment manufacturer and chemical manufacturer. Rinse the item with distilled water and dry with a lint-free cloth.
Always follow the manufacturer’s recommendations for the use of a disinfectant including contact times.
Spray bottles are not a suitable method for disinfecting equipment because:
the droplets produced do not come into contact with all parts of the equipment
droplets in the air unnecessarily expose staff to the dangerous chemicals.
Immediately discard chemical disinfectant solutions used for soaking items
Do not top disinfectant solutions with fresh solution.
Disinfection is not a sterilisation process. Wherever possible, sterilise items to be used for semi-critical or medium-risk sites, or use sterile single-use items.
Note:
Wiping instruments with disinfectants just prior to use does not provide adequate high-level disinfection or sterilise them.
Instruments should not be stored in disinfectants (before or after cleaning) as some disinfectants are corrosive and can damage equipment.
Suitable disinfectants for non-immersible items
Suitable disinfectants for non-immersible equipment are those with the following strengths:
70 per cent w/w ethyl alcohol
80 per cent v/v ethyl alcohol
60 per cent v/v isopropyl alcohol
Wipe over non-immersible items with the alcohol solution. Allow the alcohol to evaporate – do not wipe off the alcohol. Store the item dry.
Observe the use-by dates on all disinfectants, including those on decanted containers.
Note:
Items that cannot be immersed must not be used as semi-critical (medium risk) or critical (high risk) instruments as they cannot be appropriately disinfected or sterilised. They may only be used as a non- critical (low risk) instrument.
Sterilisation of reusable instruments and equipment
Sterilisation makes an item free from all forms of viable microorganisms.
Unless items are processed under controlled conditions, they will have microorganisms on them and will, therefore, be non-sterile.
The purpose of sterilisation is to destroy all of these microbiological contaminants. Sterilisation may be achieved by heat, chemicals or ionizing radiation.
Office-based facilities can use two methods of sterilisation: steam under pressure (steam sterilisation) and dry heat.
All sterilisers must be listed on the Australian Register of Therapeutic Goods (with the TGA). When purchasing a steriliser ensure the product complies with this requirement.
Dry-heat sterilisers
Although you may use a dry-heat steriliser in your hair, beauty, tattooing or skin piercing business, this type of steriliser has limitations.
Dry heat requires very high temperatures (160–180 degrees Celsius) and considerable time (for example, a holding time of 120 minutes) to achieve sterilisation.
The high temperatures required may damage materials.
For this reason, we do not recommend using a dry-heat steriliser in your business.
Steam sterilisers
Steam sterilisation under pressure is the most reliable way of sterilising reusable instruments in hair, beauty, tattooing and skin penetration businesses.
Small steam sterilisers are usually called ‘bench-top’ or ‘portable’ sterilisers.
The relevant Australian Standard for reprocessing of reusable instruments for the hair, beauty, tattooing and skin penetration industries is ‘AS/NZS 4815:2006 Office-based health care facilities – reprocessing of reusable medical and surgical instruments and equipment, and maintenance of the associated environment’. If sterilising your own items, you should comply with this Standard.
The following equipment will not sterilise items. Do not use any of these items for this purpose.
microwave ovens
pressure cookers
incubators
ultraviolet cabinets
boiling-water units
ultrasonic cleaners
household ovens
other similar units, such as pie warmers
dishwashers
glass (heat) bead ‘sterilisers’
‘steam sterilisers’ for babies’ bottles and equipment (electric or microwave versions).
Unless your staff have adequate training in the sterilisation process, we recommend you purchase sterilisation services from an appropriate local provider. Alternatively, you can use pre-sterilised single- use items so you do not need to sterilise your own items.
Cannulated items and reusable tubing
These items and tubing can be difficult to sterilise. Air or water may be trapped in cannulated items and tubing during the sterilisation cycle.
Any air remaining in the steriliser chamber or cannulated items/tubing will prevent effective sterilisation, leading to sterilisation failure.
Water remaining in reusable tubing will wet the packaging, rendering the tubing non-sterile. We recommend using single-use tubing.
Part C: Procedure-specific requirements
The principles outlined in Part B are the basis of all the following procedures.
Note:
The cleaning or reprocessing requirements in these sections is the minimum level of reprocessing required.
If a non-skin penetrating instrument or piece of equipment accidentally penetrates the skin or becomes contaminated with blood, it should be disposed of or cleaned and sterilised before being re-used.
Hairdressing and barbering
Hairdressing includes services such as hair shampooing, cutting, colouring and styling. Barbering businesses may also include beard trimming and face-shaving services.
Key points for business proprietors
Hairdressing and barbering pose a low risk for transmission of infection.
Using razors and scissors presents a small risk of transmission of blood-borne viruses.
Razors should be single-use only.
We do not recommend using electric shavers as they can become contaminated the same way that razors can.
Specific health-risk information
Although infections can occur during hairdressing and barbering procedures, in general they pose a low risk for transmission of infection.
Infections that can be spread in hairdressing premises include skin infections on the scalp, face and neck such as impetigo (also known as school sores) and fungal infections such as tinea capitis and ringworm.
These infections can spread when you do not clean instruments and equipment between clients, when you do not handle instruments hygienically, and when things like furnishings and fittings are not kept clean and in good repair.
Pediculosis or head lice are common and often cause concern. Head lice are spread through direct hair- to-hair contact. Head lice do not have wings or jumping legs so they cannot fly or jump from head to head. They can only crawl. Head lice do not transmit any infectious diseases and there is no evidence to suggest that the environment is of significant concern in their transmission. Infection in wounds caused by scratching may occasionally occur. While there is no regulation preventing a person with head lice or their eggs from using or attending a hairdressing salon, you may ask someone to reschedule their appointment. Although head lice only survive on the human head, all hair dressing equipment should be washed and dried before reuse. Lice are easily killed by water temperatures greater than 60
degrees Celsius. No disinfection or fumigation of the salon is required.
There is a small risk of transmission of blood-borne viruses through the use of razors and scissors. Razors should be single-use only. If other items such as scissors are contaminated with blood or body fluids, you should clean and sterilise them before reuse, or disposed of them if they cannot be sterilised.
You should ask clients if they have any skin lesions such as prominent moles. Ask the client to specify the location so you can take care to avoid damaging them.
Electric shavers are considered contaminated with blood after use in the same way that other razors and blades are contaminated. The blades, mesh and the blade mechanism housing are difficult to clean and will not withstand the sterilisation process. This difficulty is due to their design and the materials they are made from. Debris from shaving, such as blood, hair and skin cells, have been found in the body and motor of electric razors. We do not recommend using electric shavers on clients, and you should not lend electric shavers to clients.
WorkSafe Victoria provides an occupational health and safety risk assessment tool in the Guide to the management of hazardous substances in the hairdressing and beauty industry, 2nd edition, June 2017.
Cosmetic application including eyelash tinting and spray tanning
Cosmetic application involves applying temporary cosmetics or make-up such as lipstick, mascara and eye shadow.
Semi-permanent make-up or cosmetic tattooing, such as eyebrow feathering, that involves skin penetration or tattooing are not discussed in this section.
Key points for business proprietors
Make sure you thoroughly clean all make-up brushes and applicators between clients.
Use only single-use sponges.
Do not apply make-up if a client has an open sore.
Dispense products from larger multi-use containers into smaller single-use containers.
Specific health-risk information
Skin infections, such as impetigo and herpes (cold sores), can be easily spread via contaminated hands and equipment. It is essential that all make-up brushes and applicators are thoroughly cleaned (washed in warm water and detergent) between clients to ensure there is no cross contamination between clients. Sponges, due to their porous nature, cannot be cleaned or disinfected adequately between clients. We recommend using single-use sponges.
Do not apply make-up if a client has open weeping sores. The risk of transmission of infection is much greater when there are actively infected sores or wounds present.
Dispense products to be used on a client from larger multi-use containers into smaller single-use (or washed and dried reusable) containers or use a single-use spatula to ensure there is no contamination of the original product
Spray Tanning
Spray tanning should be conducted in a well-ventilated room, this includes recirculating and filtered air booths to avoid respiratory problems.
All surfaces in the tanning booth and treatment room should be smooth and washable, and cleaned at least weekly to remove excess tanning solution that may harbour microorganisms.
Give clients:
disposable panties
eye protection.
Staff should use appropriate PPE. This includes:
a single-use P2 respirator
a disposable apron
eye protection.
PPE should be single-use and disposed of after each client. If reusable (for example, eye protection), the item should be cleaned between uses, particularly if worn by more than one staff member.
Eyelash tinting
Eyelash tinting involves applying dye to the eyelashes. Care should be taken when applying any products to the eyelashes to avoid product or chemicals getting into the eyes.
Ensure all equipment has been thoroughly cleaned between clients in order to avoid the spread of infections such as conjunctivitis.
Clients with any signs of eye-related infection should have their treatment postponed until the infection has cleared.
Hair removal
There are several ways hairs are removed in the beauty therapy setting. These include:
waxing
plucking
threading
sugaring
electrolysis
laser or intense-pulsed light (IPL)
Laser and IPL are also used for other cosmetic treatments.
Waxing is a common method of temporary hair removal. Waxes are supplied in several forms, with different methods of application and use employed for each type of wax. Different types of waxes include glucose-based (water-soluble) wax, soft wax and hard wax.
Application methods also vary according to the type of wax used. These can include roll-on or spatula applicators (for example wooden ‘ice-cream’ sticks).
Whichever waxing product or method is used, you must maintain basic principles of infection prevention.
Plucking (for example tweezers) and threading are other methods of hair removal that may be used for smaller areas (for example eyebrows).
Key points for business proprietors
The risk of infection from waxing is very low.
Clean the area to be waxed with a skin antiseptic.
Use a single-use pot for each client.
If you use a multi-use container, use a new spatula each time you dip it into the wax.
Do not apply wax to broken skin or if the client is bleeding.
Specific health-risk information
Waxing
Although the risk of infection associated with waxing is very low, you should still take steps to reduce the risk further.
Before waxing a client, clean the area of skin with a skin antiseptic. This will reduce the levels of skin bacteria and the risk of skin infection.
To prevent cross-contamination between clients, use either of the following two methods for wax application.
Use a single-use pot for each client. Clean the pot thoroughly after each client.
If using a multi-use container, never double-dip into wax. Use a new spatula each time. We recommend using disposable single-use wooden spatulas.
However, if neither of these methods is practical, you must use temperature control to minimise possible risk.
Keep types of wax (both strip and hot wax) undisturbed at a minimum temperature of 70–80 degrees Celsius for a minimum of 15 minutes between clients. (Generally, viruses such as HIV are inactivated at this temperature.)
For strip waxing, monitor temperature and record it before the first client and at least one other time during the day.
For hot waxing, monitor temperature between clients, or at least twice during an eight-hour day.
For both strip and hot wax, monitor temperature after pots have been refilled or replaced with a new pot.
You should keep records of temperature and time of holding make them available for inspection for a reasonable period (at least one year).
Do not apply wax to broken skin or over an area where blood has been drawn. If wax and/or instruments are contaminated with blood, use the following procedures:
Immediately discard wax into the clinical and related waste container.
Discard wooden applicators into the clinical and related waste container.
Discard metal applicators or tweezers into a sharps container, or clean and sterilise them before using them on another client.
Take special care when removing hair from the upper lip, underarm or pubic area. These areas are either moist or close to mucous membrane areas, which are more sensitive and support a higher level of microorganisms.
Do not re-use hot hard wax between clients.
Roll-on applicators
Where possible, we recommend using roll-on applicators that can be dismantled and thoroughly cleaned between clients. Applicators that cannot be dismantled may not be able to be adequately cleaned and disinfected between clients.
Place wax cartridges with their roll-on applicators attached in an enclosed heating unit capable of heating the wax cartridge and roller head to a temperature level of 70–80 degrees Celsius for a minimum of 15 minutes between each client.
Plucking
Plucking is more likely to cause bleeding than other hair removal processes. Instruments must be cleaned and disinfected after each client, or cleaned and sterilised if contaminated with blood.
Threading
Threading involves pulling hairs from the follicles using a thread that is moved quickly over the skin, catching the hairs and causing their dislodgement from the follicle. Threads must be used only once and then discarded.
Sugaring
Sugaring involves the use of a thick sugar-based paste which is spread onto the skin and then removed using the hands to ‘roll’ it against the hairs to remove them.
Sugar-based pastes provide an ideal environment for potentially harmful organisms to grow. As such, you must make sure the original product does not become contaminated.
Wash your hands or use an alcohol-based hand rub and put on a new pair of gloves each time you remove a portion of sugar-based paste from the original container.
Electrolysis
There are three types of electrolysis used to remove unwanted hairs:
Thermolysis uses radio waves to generate heat. This destroys the papilla (blood supply) and prevents it from feeding the bulb, stopping the follicle from producing more hairs.
Electrolysis uses a direct current (galvanic). When applied through the probe, the current produces a chemical called ‘lye’, which destroys the growing cells and the papilla.
A combination of the two types can also be used.
All three methods are applied by passing a fine probe down the hair follicle without breaking the skin. When the probe is in position, the correct amount of one or both currents is applied.
Blood-borne viruses and other infections may occur during electrolysis because the electrically heated needles inserted into hair follicles can become contaminated with blood.
To reduce the risk of infection, use only sterile single-use needles. Sterile, single-use needles are inexpensive and readily available, there is no need to re-use electrolysis needles. You can use one needle for removing as many hairs as necessary from one client during one session, but the needle should be sterile at the first time of use. Dispose of the needle into an approved sharps container immediately after use.
Facials
Facials include a broad range of skincare treatments such as steam, exfoliation, extraction, creams, peels and massage. Light treatments such as LED and laser may also be used
Key points for business proprietors
Clean the client’s face before you give a facial massage or apply any products.
Do not provide a facial massage if the client has open sores.
Dispense products from multi-use containers into single-use containers.
Specific health-risk information
Clean the client’s face before a facial massage or applying any products. Do not conduct a facial massage if the client has open, weeping sores. The risk of transmission of infection is much greater when there are actively infected sores or wounds present.
Dispense products to be used on a client from larger multi-use containers into smaller single-use containers or use a single-use spatula to ensure there is no contamination of the original product
Eyelash extensions
Eyelash extensions are semi-permanent extensions adhered to the natural lash. Two types of artificial lashes are commonly used.
Strip lashes are eyelash hairs on a band that are applied to the natural lash line.
Individual lashes are separate artificial lashes that are applied to the base of the individual natural eyelash.
Lashes can be made from a variety of different materials, including synthetic, mink and sable, or silk. Adhesive is used to make the artificial eyelashes adhere.
Key points for business proprietors
Clients can have an allergic reaction to adhesives or dyes. The client may wish to test the product on their skin at least 24 hours before the procedure.
Use an aseptic non-touch technique (see p. 27).
Dispense product from larger containers into single-use containers.
Specific health-risk information
The adhesives and dyes you use must be fit for purpose.
Allergic reactions are the most common risk. If the client is unsure or thinks they may have a reaction, they may wish to test the adhesive or dye on their skin at least 24 hours before the procedure.
Applying eyelash extensions may also spread conjunctivitis or other skin infections. Use an aseptic non- touch technique to ensure the artificial eyelashes are not contaminated before or during the procedure.
Dispense products (for example, eyelashes or glue) to be used on a client from larger containers into a smaller single-use (or cleaned and dried reusable) container to ensure there is no contamination of the original product.
Manicure, pedicure and nail treatments
Manicures and pedicures include filing and shaping of nails, exfoliation of dead skin, moisturising and massage.
Key points for business proprietors
The risk of infection from manicure, pedicure and nail treatments is generally low. However, poorly cleaned, disinfected or sterilised instruments can lead to serious infections.
Maintaining good hygiene and taking sensible precautions can reduce the risk of infection.
Clean and dry the client’s hands or feet before the procedure.
Use first aid if you cut or injure the client. The wound may become infected from their own normal flora (microorganisms).
Specific health-risk information
Fungal infections can cause tinea or ringworm, affecting hair, skin and nails.
Paronychia (infection of the nail folds) can be caused by Candida albicans (a form of yeast infection) and bacteria such as Staphylococcus aureus and Streptococcus pyogenes (group A streptococcus).
If the bacterium causes cellulitis (a spreading infection below the surface of the skin with redness, warmth, swelling and pain), then it can cause severe damage and become serious very quickly.
Fungi more commonly infect toenails than fingernails. Less than 10 per cent of nail infections involve fingernails.
It is important that you do not perform work on nails that are abnormal in appearance or have any sign of infection (redness, pus, tenderness or swelling). You should not cover up infected nails. Advise the client to consult a medical practitioner.
When acrylic nails and similar products are attached to normal nails, avoid leaving any space between the natural and acrylic nail. These spaces provide the perfect environment for microorganisms to grow.
Pedicures can present more potential for damage and infection to clients than manicures. Before conducting a pedicure, ask the client if they have any health conditions (for example, diabetes), which may place them at a greater risk of infection or complication.
You should also check the client’s skin integrity. Do not perform a pedicure if there are any signs of broken skin (for example, blisters) or infection (for example, tinea).
You may use items such as nail files and buffers on one client for a period of time, however equipment should be stored in an appropriately labelled container, for example, a zip-lock plastic bag with the client’s name on it. These items will still need to be cleaned between uses and stored dry.
Information regarding the safe use and management of hazardous substances used in nail products can be found in the Guide to the management of hazardous substances in the hairdressing and beauty industry, edition 2, June 2017.
Foot spas
Foot spas (foot baths with a whirlpool action or water jets) have been associated with a number of bacterial outbreaks, particularly non-tuberculous mycobacteria. Poor cleaning and disinfection practices lead to a build-up of organic debris in the filters and jets, allowing microorganisms to multiply and recirculate in the footbath water.
A single-use disposable foot spa liner can be used for each client. Otherwise, the foot spa must be drained, cleaned and disinfected between each client and at the end of each day. See below for links to examples of instructions for cleaning and disinfection of foot spas.
Dry needling and other therapeutic skin penetration procedures
Dry needling uses a solid, filament needling technique. It is used by myotherapists, physiotherapists or osteopaths, and is different from the acupuncture techniques used by Chinese Medicine specialists. The theory, clinical reasoning and application behind the two techniques is different.
Acupuncturists who are registered with the Chinese Medicine Board of Australia under the Health Practitioner Regulation National Law are exempt from the requirement to register their business with local council.
Although physiotherapists and osteopaths are also required to be registered with AHPRA, they have not been provided with an exemption from registering their business if they undertake skin penetration procedures under the Public Health and Wellbeing Regulations (2009) (see r. 15 for the full list of health professionals and businesses exempt from the requirement to register their business).
If you are a physiotherapist or osteopath who performs dry needling, you must register your business with your local council.
In some instances, other physical therapists who are not registered with AHPRA, for example myotherapists, may also perform dry needling or other therapies that involve skin penetration procedures, for example wet cupping. If you perform skin penetration procedures in this type of healthcare business, you must register your business with the local council.
Key points for business proprietors
The risk of infection from dry needling is low.
You should ensure the skin is clean and free from oils. You may need to wash the skin.
Disinfect the skin before any skin penetration procedure.
Specific health-risk information
The skin surface should be clean and free of emollients or oils.
You may need to wash the area with soap and water prior to a treatment.
Although the risk of infection is low from these types of therapies, particularly from very fine acupuncture- type needles, you should disinfect the skin prior to any skin penetration procedure
Laser and intense pulsed light (cosmetic procedures and tattoo removal)
Both laser and intense pulsed light (IPL) use light to perform skin treatments such as, hair removal, treatment of skin pigmentation and blemishes, and tattoo removal.
Lasers work by producing a beam of light that has a single wavelength (monochromatic). The beam of light can be focused on the area to be treated.
Lasers are classified according to ‘AS/NZS IEC 60825.1:2014 Safety of laser products, Part 1: Equipment classification, requirements’. There are several classes and types of laser available.
Lasers used for cosmetic purposes are usually classes 3B and 4. Each poses a different level of risk to both clients and staff. You must make sure equipment is used safely.
Lasers are sold under various names and you should ask for clear information related to the type/class of laser you are considering, including safety information.
Registered premises operating lasers should follow ‘AS/NZS 4173:2018 Guide to the safe use of lasers in health care’ and ‘AS/NZS IEC 60825.14:2011 Safety of laser products, Part 4: A user’s guide’.
IPLs work by producing intense pulses of light over a range of wavelengths. The light produced can be filtered and manipulated by the machine to make its effects more specific.
Key points for business proprietors
Staff need to undergo training before they can use any type of laser or IPL device.
Lasers and IPLs can be dangerous. They can burn, blister or scar the client. They can cause eye damage.
Staff and clients should wear PPE.
Different devices have different cleaning and disinfection requirements.
Specific health-risk information
Lasers and IPLs used for cosmetic purposes can be hazardous. Clients have been injured following use of laser or IPL for cosmetic procedures. Injuries include burns, blistering, scarring, increased or decreased skin pigmentation and eye damage.
Rooms in which lasers are used should be designed for the purpose. Clients and staff should wear PPE, including gloves, single-use face masks suitable for the purpose and eyewear that meets the standard for use with lasers.
Lasers/IPLs used for cosmetic purposes are usually self-contained units that need minimal cleaning and sterilisation.
The end where the laser/IPL beam emerges should not come into contact with the client. However, it may become contaminated via the dispersal of contaminated tissue including body hair.
There are devices with ends that can be removed for cleaning and sterilisation. Some devices can be used with a protective cover (sheath) to reduce contamination. We recommend using single-use sheaths or protective covers for procedures where there is a high likelihood for skin damage, for example tattoo removal. You will still need to reprocess the laser/IPL device in the usual way.
Cleaning and disinfection of lasers/IPLs will depend on the type of device used. Devices with end pieces (of the laser/IPL arm) that can be dismantled should be cleaned after each client. If the skin is damaged (broken) during the procedure, the arm is likely to be contaminated with blood or body fluids and should be cleaned and sterilised after use. Devices that are self-contained (that is, the arm cannot be dismantled) should be cleaned and disinfected as for non-immersible items
The Australian Radiation Protection and Nuclear Safety Agency (ARPANSA) have developed nationally- available advice for the cosmetic and beauty therapy industry to promote a uniform approach to managing key issues around the use of light-based devices for non-surgical cosmetic treatments.
Information for consumers and providers of lasers and other light-based cosmetic therapies can be found at the following websites.
Tattooing (including cosmetic tattooing)
Tattooing is a very popular form of body art. It involves injecting ink into the dermal layer of the skin to permanently or semi-permanently colour the skin for body art or cosmetic purposes. Semi-permanent cosmetic tattooing includes microblading or feathering.
Tattoo inks consist of a colourant combined with a carrier. Colourants used may be pigments that are insoluble in water or dyes which are soluble in water. Frequently heavy metals such as mercury, lead or cadmium are used in pigments as well as metal oxides or other elements such as carbon or arsenic. A carrier acts as a solvent to keep the ink evenly mixed and aid in application. Carriers include water, glycerol, propylene glycol, alcohols (isopropyl or methyl alcohol) and witch hazel.
Key points for business proprietors
Preventing contamination of tattoo inks is very important.
Dispense inks into sterile containers or caps.
Request a product quality data sheet when you buy inks to confirm the product is safe and legal to use in Victoria.
Use an aseptic non-touch technique (p. 27).
Open sterile items in front of the client so they know you are using sterile instruments.
Clean and disinfect skin before tattooing.
Specific health-risk information
The most common complications from tattooing are skin infections and allergic reactions to the ink. Outbreaks of skin infections caused by Mycobacterium chelonae, a non-tuberculous Mycobacteria
(NTM), in New York State, USA were associated with contaminated tattoo ink. Investigation of this and other NTM clusters of infections by the Centers for Disease Control and Prevention (CDC) found all were related to inks likely contaminated by the use of non-sterile water in either the manufacture of the inks or during dilution by the tattoo artist just prior to use on a client.
Preventing contamination of tattoo inks is very important. Do not use inks or other products that are not intended for tattooing. Use an aseptic non-touch technique to dispense inks into pre-sterilised containers or caps before working on a client. If inks require dilution only use sterile water and discard any leftover inks. Use sterile water to rinse equipment (for example, needles) during tattooing.
It is your responsibility to ensure you request a product quality data sheet (certificates of analysis or an equivalent statement) when purchasing inks from suppliers or directly from manufacturers to confirm that the product is safe and legal for use in Victoria. You should ensure, for each substance you intend to use, the tattoo ink is correctly labelled and does not contain anything that should not be used for tattoos.
You can prevent transmission of blood-borne viruses using standard precautions. Use an aseptic non- touch technique to set up the work area and equipment. At the end of a tattoo session, dispose of all
contaminated items, waste and leftover products.
Open all sterile items in front of the client to show them you are using sterile instruments. Check the chemical indicators for colour change and, if satisfactory, assemble the handpiece. Replace any sterile instruments or needles you accidentally touch or contaminate in any way, either before or during a treatment, with another sterile instrument or needle. If more ink or other items are required during a procedure, remove gloves and perform hand hygiene before dispensing or opening other items.
Ensure the client’s skin is clean and free from infection, sores or wounds on or around the tattoo site. If the tattoo area needs to be shaved, use a new single-use safety razor for each client. Disinfecting skin prior to tattooing will also decrease the risk of skin infections
Body piercing and other forms of body modification
Body modification is the deliberate altering of a person’s physical appearance. Many forms of body modification have been practiced throughout history by many different cultures. Body piercing (for example, ear or nose piercing) is one of the most common forms of body modification.
Other forms of body modification include:
scarification – cutting skin with a scalpel or laser to produce scarring. Foreign matter, such as clay or ash, may be inserted or rubbed into the wounds to achieve permanently raised welts or keloid scarring
branding – using a hot or very cold branding iron to produce scarring
braiding – cutting adjacent strips of skin (one end remains attached), braiding the strips of skin together, then reattaching the ends to the skin
beading – implanting foreign objects beneath the skin, such as beads, rings or other shapes.
Note:
It is against the law to:
perform scarification, tongue splitting, branding, beading and intimate body piercing on anyone under the age of 18 years
perform non-intimate body piercing on someone under the age of 16 years without the consent of a parent or guardian
allow a person under the age of 16 years to perform intimate body piercings.
Key points for business proprietors
Use aseptic non-touch technique (p. 27).
Clean and disinfect the client’s skin before the procedure.
Use single-use instruments where possible.
Specific health-risk information
Common complications of body piercing and other body modification procedures include:
localised or systemic infection
excessive scarring (for example, keloid)
excessive bleeding
reactions to the material inserted for piercings or implantations.
You can significantly reduce the risk of infection by using aseptic non-touch technique and appropriate antisepsis of the skin before piercing or cutting the skin.
Using disposable single-use instruments also significantly reduces transmission of blood borne viruses.
To minimise the chance of the client having a reaction to the metal in body-piercing jewellery, use jewellery manufactured from surgical stainless steel (nickel free), titanium, niobium or similar inert metals.
Under the Public Health and Wellbeing Regulations 2009 (r. 32), you must give the client accurate, written information about the transmission of infectious diseases associated with the process.
Use of local anaesthetic
Topical anaesthetics like EMLA 5 per cent cream (lidocaine/prilocaine) are Schedule 2 poisons or Pharmacy Medicines. They can be bought at a pharmacy without a prescription. If you are using a topical anaesthetic, the client should buy their own tube from a pharmacist and use it as required.
Injectable anaesthetics, for example ropivacaine, are Schedule 4 poisons or ‘Prescription Only Medicines’. Schedule 4 medicines can only be prescribed by a registered medical practitioner and be administered by a registered medical practitioner or a registered health practitioner (such as a nurse) under the instruction of a registered medical practitioner. Injectable anaesthetics cannot be used by non- medical proprietors and staff.
Colonic irrigation
Colonic irrigation is also known as colonics, colonic lavage, colon irrigation, high colonic or colon hydrotherapy. The practice involves cleansing the entire colon from the rectum to the caecum through the administration of water, herbal solutions, enzymes or other substances such as coffee.
Colonic irrigation differs from the enema currently used in the healthcare environment. Enemas use small amounts of electrolyte-based solutions to clean the bowel before surgery and to assist in faecal disimpaction procedures.
Colonic irrigation can be administered via an open or closed system. Both involve insertion of a catheter or speculum into the rectum and gravity or pressure-fed water to flush the contents of the colon. In an open system the catheter inserted is small and only used to flush water into the bowel. The water and faecal matter then drain away freely, usually into the sink of a specifically designed table. In a closed system a speculum is inserted, and a small catheter attached for water to flow into the bowel and a larger tube attached to drain away the water and faecal matter.
Key points for business proprietors
Seek consent of your local water authority before installing equipment.
Use a licensed plumber to install equipment.
Follow the manufacturer’s instructions and recommended maintenance procedures.
Colonic irrigation equipment must not be directly connected to mains water. This can be dangerous for the client.
Clients should not be able to alter control settings once the procedure commences.
Use single-use tubing where possible. Reusable tubing is difficult to clean, disinfect and sterilise.
Specific health-risk information
Equipment
Colonic irrigation equipment is a medical device. It should have an Australian Register of Therapeutic Goods (ARTG) inclusion number (listing or registration). You should have policies and procedures for safe operation in place, and you should follow the manufacturer’s instructions, including maintenance procedures.
Under no circumstances should the colonic irrigation equipment be connected directly to a potable water supply system. A direct connection could result in a serious (and possibly fatal) injury to a client due to
application of mains pressure, and if there is a sudden drop in mains water pressure, the potable water supply could become contaminated with faecal material.
The following practices are also important:
Place controls so clients cannot alter settings once the procedure commences.
Use suitable water filters (1–20 microns filtration) on all systems to reduce/remove particulate matter. Filter water before it enters the storage tank. Replace filter elements as per manufacturer’s instructions and as necessary. (It may also be necessary to install a pump to ensure adequate water flow to the storage tank.)
For a gravity-fed system, the minimum vertical distance between the top of the couch and the tank outlet spigot should be 650 millimetres. The maximum distance between the couch top and the upper level of water in the feed tank should be 1,300 millimetres.
There should not be pumps, other pressure-enhancing devices or suction facilities on the client side of the tank. Mechanisms for regulating water temperature should be installed at the mains and the tank.
Reusable tubing poses a challenge to cleaning processes. Cleaning processes can generate infectious droplets in the air (particularly given that tubing is difficult to sterilise). If equipment tubing needs lubrication, moistened each end with water before connection.
If you use UV light, it should be fitted with screening to protect the client, because it can damage the skin and retina.
Catheters
Catheters should be sterile and single-use only. You should only purchase items that are on the Register of Therapeutic Goods, and you should ask suppliers for the ARTG number.
Single-use tubing is recommended as per Section 2.7 (p. 18) of AS/NZS 4815:2006. Cleaning and sterilisation of tubing is problematic, so you should use single-use tubing.
Reprocessing reusable tubing can create infectious droplets in the air. Reusable tubing is difficult to clean and sterilise. It is hard to completely remove air from tubing. If air remains in the tubing, steam cannot penetrate the lumen and the tubing will not be sterilised.
Plumbing/sewage disposal
You should seek the consent of the local water authority before you install any colonic system. Installation should conform with the standards of the Plumbing Industry Commission (Victoria) and Standards Australia (see below).
Show the following Australian Standards to a licensed plumber to ensure compliance.
AS/NZS 3500.1:2015 Plumbing and drainage – Water services
AS/NZS 3500.2:2015 (incl. Amdt 1:2017) Plumbing and drainage – Sanitary plumbing and drainage
AS/NZS 3500.4:2015 Plumbing and drainage – Heated water services.
For practices that will be in areas where a non-potable water supply and/or non-mains sewage system is to be used, for example on a rural property with a private water supply and septic tank system, seek council advice before registration to ensure you comply with local requirements.
The following practices are also important.
Treatment beds connected to either a water supply or sanitary plumbing system should be authorised and certified prior to being installed in a plumbing system.
All plumbing should be easily accessible.
The system should be odourless and prevent backflow to, and subsequent contamination of, mains water.
A reduced pressure zone device should be fitted on the water supply line to the colonic equipment.
Water authorities may also require a reduced pressure zone device to be fitted at the water meter outlet to contain any possible backflow within the property.
The storage tank should be vented to atmosphere. Gravity-fed tanks create a physical air gap, known as a registered air break, to prevent backflow.
The treatment bed should be equipped with non-return and pressure-reducing valves to prevent backflow of faecal material.
Waste should be removed by the installation of flushing-floor waste in lieu of normal floor waste.
All waste should be discharged to a sewer, and there should be approval for this connection.
A pressure hose should be available to clean the system.
Hot water installations should deliver water at the outlet of all sanitary fixtures used primarily for personal hygiene at a temperature to ensure scalding does not occur.
Hot water is to be stored at 60 degrees Celsius to inhibit the growth of Legionella bacteria.
Note:
Legionella is not a transmission risk during colonic irrigation procedures, but it may be during tank cleaning if aerosols are present.
Water temperature should be regulated to normal body temperature to prevent thermal shock or scalding. The temperature of the water delivery should be 34–40 degrees Celsius and should never exceed 40 degrees Celsius. Normal body temperature (37.6 degrees Celsius) should be the guide.
A water-based lubricant in a single-use sachet is recommended to assist catheter insertion. If the client is positioning the catheter, then they should be provided with single-use gloves and moist wipes. Care should be taken to avoid cross-contamination.
Clients should seek medical advice before undertaking any colonic irrigation procedure. Potential risks for clients include:
infection due to inadequately cleaned and disinfected or sterilised equipment
infection due to equipment that permits backflow of faecal material to and from the water system
trauma to the colon or exacerbation of bowel diseases
thermal shock or scalding if regulation of the water temperature fails
a reduced capacity to control bowel movements for a period of time after the procedure
a change in bowel flora, which may lead to such problems as gastrointestinal infections.
The operator/therapist should wear appropriate PPE to avoid contamination of clothing or splashes to face and eyes
Disinfectants
Disinfectants should be used in colonic irrigation premises for the couch, the external irrigation system and ensuite facilities due to the high risk of faecal contamination.
Use a disinfectant registered or listed with the TGA as a hospital-grade disinfectant that is effective against norovirus and Clostridium difficile spores. Sodium hypochlorite (bleach) at a minimum of 1,000 ppm is generally the best disinfectant for this purpose for routine disinfection of surfaces.
Sodium hypochlorite is corrosive on some materials, particularly metal. After the appropriate contact time required for disinfection (usually 10 minutes), you should rinse or flush surfaces or equipment to remove any bleach residue.
Part D: Occupational health and safety
Quick guide for business proprietors
This quick guide provides an overview of the main points of occupational health and safety for your business.
The quick guide may not contain everything you need to know to meet your legal obligations. Use the page references to find out more about each topic.
Provide a safe working environment (p. 76)
It is your responsibility to provide a safe working environment for staff and clients.
Vaccination (p. 76)
Staff who perform skin penetration and tattooing, or who clean instruments and equipment, should be
vaccinated for hepatitis B.
Staff who perform colonic irrigation should be vaccinated for hepatitis A.
Exposure to blood or body fluids (p. 76)
All staff need to know how to prevent exposure to blood and body fluids, Staff also need to know what to do if they are exposed.
First aid (p. 77)
All staff should be trained in first aid for the types of injuries that may occur in your business.
For example, if you provide waxing services, staff should know what to do if someone is burned by hot wax.
Chemicals (p. 77)
You must store and use chemicals safely.
Providing a safe work environment
You are responsible for providing a safe work environment to minimise risks to the health of employees, clients and other people entering the premises. The Occupational Health and Safety Act 2004 and Occupational Health and Safety Regulations 2017 set out the key principles, duties, rights and obligations of all employers and employees.
This involves providing:
adequate staff training, including training in infection prevention and control
properly maintained facilities and equipment, including personal protective equipment
a suitably designed and clean workplace to minimise potential hazards, such as the safe storage of equipment and chemicals, sharps and other clinical and related waste.
This can be achieved through a good understanding of these guidelines and their application.
Vaccination
Vaccination for hepatitis B is recommended for all staff involved in skin penetration and tattooing procedures, and for staff involved in cleaning instruments/equipment.
Hepatitis A vaccination is recommended for staff working in colonic irrigation premises. Vaccination can be arranged through a general practitioner.
Occupational exposure to blood or body fluids
The blood and body fluids of all persons are to be considered potential sources of infection, regardless of perceived risk.
Transmission of blood-borne viruses may result from percutaneous exposure (‘sharps’ injury) or mucocutaneous exposure (‘splash’ exposure).
The risk of acquiring hepatitis C, hepatitis B or HIV depends on the amount of blood/body fluid the person is exposed to, and the method of exposure (that is sharps injury vs splash exposure).
All staff need to know how to prevent exposure to blood and body fluids, and what to do in the event of a blood or body fluid exposure.
Management of blood or body fluid exposures
Intact skin
There is no evidence that blood-borne viruses can be transmitted by blood or body fluid contamination of intact skin.
If blood or body fluids come into contact with intact skin, wash the area thoroughly with liquid soap and warm water and dry with paper towel.
Non-intact skin
If blood or body fluids come into contact with skin that is chapped, cut or abraded, or has dermatitis, or if accidental penetration (for example, a sharps injury) occurs, you should:
Allow the wound to bleed (if a puncture wound) and wash the area with soap and warm water. There is no need to squeeze a puncture wound to promote bleeding.
Thoroughly pat the area dry with paper towel.
Cover the wound with a waterproof dressing.
Apply firm pressure to control bleeding if required.
Mucous membranes (eyes/mouth)
If blood or body fluids come into contact with mucous membranes, you should:
for eyes, rinse gently with eyes open, using plenty of tap water or saline solution
for the mouth, spit out the blood or body fluid, then rinse the mouth thoroughly and repeatedly with warm tap water.
Follow-up action
Report the incident to the proprietor or manager of the business immediately. Go to a general practitioner.
You should also write down:
The name of the exposed individual.
The date and time of exposure.
How the incident occurred.
A description of the injury and treatment provided.
The name and contact details of the individual who is the source of the blood or body fluid (if known).
A general practitioner should evaluate all exposures as soon as possible for both the source individual and the person exposed.
First aid
All premises should be aware of the types of injuries that may occur as a result of the procedures the business undertakes, for example burns due to hot wax or chemicals.
Staff should be appropriately trained to manage these types of injuries. You should provide easily accessible information on how to treat injuries.
Further information on first aid basics can be found at the Better Health Channel.
Use and storage of chemicals
Many chemical products used in the hair, beauty, tattooing and skin penetration industries have the potential to harm staff and clients if they are not used appropriately.
It is beyond the scope of this document to provide advice about using and storing chemicals.
However, you should ensure you ask manufacturers or suppliers of chemicals for safety data sheets (SDS) relating to the safe handling, storage and first aid requirements for all chemical products used within the business.
All proprietors of hair, beauty, tattooing and skin penetration businesses should refer to these sheets for advice, and keep copies on the premises at the point of use.
If chemicals are decanted into other containers, these containers must be appropriately labelled.
Ventilation
Part of your responsibility to provide a safe work environment includes appropriate ventilation to reduce the risk of exposure to hazardous chemicals.
An occupational health and safety risk assessment tool is provided by WorkSafe Victoria in the Guide to the management of hazardous substances in the hairdressing and beauty industry, edition 2, June 2017.
Use this assessment tool to determine additional controls required to minimise such risks.
Your business should also comply with the Australian Standards for ventilation and air conditioning in buildings.
‘AS 1668.2-2012 The use of ventilation and air conditioning in buildings – Mechanical ventilation in buildings’
‘AS 1668.2-2012/Amdt 1-2013 The use of ventilation and air conditioning in buildings – Mechanical ventilation in buildings’
‘AS 1668.2-2012/Amdt 2-2016 The use of ventilation and air conditioning in buildings – Mechanical ventilation in buildings’.
Part E: Appendices
Appendix 1: Ultrasonic cleaners
Ultrasonic cleaner method
Use the following method for ultrasonic cleaning.
Fill tank with water (temperature is not critical) and add measured amount of recommended detergent for ultrasonic use. Use only a detergent recommended by the manufacturer because others may limit the effectiveness of the ultrasonic cleaner.
Operate the machine for a short time to degas the solution.
Ensure any gross contamination is first wiped or rinsed off instruments.
Dismantle or fully open items to ensure all parts are present and to facilitate cleaning.
Place the instruments in the machine’s basket and submerge basket in the water tank.
Close the lid and commence the cycle (for length of cycle refer, to the manufacturer’s instructions).
Keep the lid on during the operation to prevent aerosols and splashing.
Remove the basket with the instruments after the specified time and rinse under warm to hot running water.
Dry items in a drying cabinet or with a lint-free cloth. Do not allow items to ‘air-dry’.
Visually inspect items for cleanliness.
Do not reassemble the items before thermal disinfection or sterilisation.
Brush cannulated items thoroughly and rinse them before placing them into the ultrasonic tank. Ensure air is not trapped inside the lumen.
Brush items again on removal (using a clean brush) to remove loosened debris. Ultrasonic cleaners do not sterilise or disinfect instruments, but they provide a safe and effective means of cleaning most reusable instruments before sterilisation.
Note:
Mechanical shaking can blunt fine points on instruments if they bump against the sides of the basket/ultrasonic cleaner.
Maintenance and monitoring of ultrasonic cleaners
Ultrasonic cleaners should be operated and maintained according to the manufacturer’s instructions. Ultrasonic cleaners should comply with ‘AS 2773.1–1998 Ultrasonic cleaners for health care facilities, Part 1: Non-portable’ and with ‘AS 2773.2–1999 Ultrasonic cleaners for health care facilities, Part 2: Benchtop’.
Check and clean base plate, gaskets, water strainers and filters daily. Conduct a performance test (follow manufacturer’s recommendations) daily to check the transducer function (for example, the aluminium foil test). Document results of the daily performance test. An unsatisfactory result indicates that the ultrasonic cleaner is not functioning at maximum efficiency, and it should not be used until it has been serviced.
Appendix 2: Steam sterilisers and the sterilisation process
Types of steam sterilisers
Sterilisers are classified according to the types of cycles they can run. There are three different types of sterilisers: Type N, S and B. They have sterilisation cycles that are linked to their intended use. That is, the type of cycle and the type of instrument being sterilised. Some more advanced sterilisers are capable of switching modes and run different classes of cycle. If a steriliser can switch modes, take care to ensure you use the correct cycle for the instruments being sterilised.
Type N cycles
These cycles do not have an active drying cycle. They are used for sterilising unwrapped solid (that is, non-lumened and non-porous) items.
Instruments sterilised in this type of cycle are intended for immediate use (which is not recommended) or for non-sterile storage. They can be used for items that need to be sterilised after use, but do not need to be sterile at the time of use.
Note:
We do not recommend using sterilisers without a drying cycle, as wrapped items cannot be processed.
Type S cycles
Sterilisers with Type S cycles have an active drying cycle. They are capable of sterilising unwrapped solid items, and at least one of the following:
porous items
Hollow load Type A or B
single and double layer wrapped items.
The following sterilisers are capable of providing Type S cycles:
gravity or downward displacement with active drying cycle
purge under pressure (assisted air removal)
single vacuum pulsed (pre-vacuum, preliminary vacuum, vacuum assisted)
multiple vacuum pulse (but not Type B cycles).
Type B cycles
These types of cycles are capable of sterilising:
all wrapped (single and double) and unwrapped items
hollow items that do not exceed the specifications of a Hollow load Type A
solid and porous items.
Type B cycles are suitable for sterilising very long, narrow, cannulated/lumened devices.
Sterilisers with a drying cycle are recommended as these can process packaged items. Premises reprocessing cannulated or lumened instruments or equipment require sterilisers with Type B or S cycles.
Sterilisers should have a sterilisation cycle process recorder/printer that monitors cycle parameters because this saves time during the sterilisation process. If a process recorder printer is not fitted, then every sterilising cycle should be monitored every 10 seconds and the time, pressure and temperature recorded. Existing sterilisers without process recorder/printers are not recommended and should be upgraded or replaced to ensure automatic parameter (time/temperature/pressure) monitoring and a permanent cycle record.
Packaging of items to be sterilised
The purpose of packaging or wrapping items for sterilisation is to provide an effective barrier against sources of contamination during storage and to allow the aseptic removal of the contents at the time of use.
The principles of packaging are as follows.
Packaging of instruments for sterilisation should be undertaken in a clean area, preferably dedicated to this purpose.
Always perform hand hygiene before packaging items to reduce the risk of contamination prior to sterilisation. Do not handle cleaned items or packaging materials after recent use of a hand cream/lotion; wash hands first.
Packages should not be overfilled.
Hollowware (bowls) should be packaged separately from instruments, with the opening facing the paper side of the laminate/paper packaging (pouches) to allow air to escape.
Items should not be too heavy for the type of packaging used, because they may break the package, particularly if they are also sharp.
The tips of sharp items should be protected to maintain sharpness and to prevent damage to packaging. Tip protectors that are steam penetrable are readily available.
Items with ratchets or toothed tip clips should not be sterilised in the locked position. Leave items open to allow steam to penetrate all surfaces.
Suitable fully perforated instrument trays may be used. Instrument trays should be inserted into the package with the contents clearly visible through the laminate side of the packaging.
If drapes are used, then they should be single-use and packaged separately from all other items. Sterile single-use drapes are available commercially.
Once packaged, care should be taken to keep these items separate from sterile items: they should be stored in a separate, clearly labelled cupboard or covered container in a dust and moisture free environment. Best practice is always to sterilise items as soon as possible after packaging.
Packaging materials
The type of packaging chosen will depend upon the:
type of steriliser used
size and contents of the packaging system (for example, laminate pouches come in a limited range of sizes)
type of reusable instrument/equipment to be placed into packaging.
Do not use rubber bands around packages (or items within packages), because air/moisture will be trapped during sterilisation. The use of rubber bands to hold sterile packages together can cause crinkling and creasing that can weaken the paper packaging and compromise sterility.
If the integrity of a sterilised package is compromised, then the items should be completely reprocessed, commencing with the cleaning process. Packages should not be re-labelled and re-sterilised.
Labelling
Packaging should be dated (date of sterilisation) and labelled prior to being sterilised. A self-adhesive label, permanent felt-tipped marker or rubber stamp may be used to label packaging. Each item being sterilised should have an identifying code for tracing steriliser faults if required. This code should be recorded on the sterilisation monitoring record.
Do not use a sharp pen (for example, ballpoint pen) because it will damage the packaging material. Water-based ink pens should not be used, because they will ‘run’ during sterilisation.
Sealing packaging
The purpose of sealing is to maintain pack integrity. You can use self-sealing pouches, heat sealers or steriliser indicator tape. Methods that compromise the integrity of the pack must not be used.
If using steriliser indicator tape to seal a package, it should be specific to the type of steriliser and compatible with the packaging material used. Fold the opening of a non–self seal bag/pouch two or three times before sealing. The indicator tape should be long enough to completely seal the front with a small fold to the back.
A heat-sealing unit may be used for sealing both laminate/paper and paper bags. Check the package seal before and after sterilisation.
Do not use staples, string, non-adhesive tape, masking tape and elastic bands as sealing agents.
Loading the steriliser
Correct loading of the steriliser is essential for effective sterilisation. Correct loading techniques:
permit efficient air removal from the chamber
allow total steam penetration and saturation of all items
allow condensate to drain
assist drying
reduce damage to packaging.
In effect, correct loading maximises efficient steriliser use. Items should not exceed the boundaries of the loading tray within the chamber and should not touch the walls of the chamber (this will bring them into contact with condensate on the chamber walls).
Tilt hollowware (bowls) on their side to permit drainage of both air and condensation during the sterilisation process. Load linen so the layers are vertical for efficient air removal and steam penetration. Do not load hollowware or instrument packages above linen, because any condensation will wet the linen/packaging, making it difficult for steam to penetrate the linen/packs and sterilise the items.
Position packages of laminate pouches or paper bags on their edge, with each package surface being paper to laminate. Use a rack to separate bags and pouches. Do not place too many packages together, because air removal and steam penetration may be compromised. They may be laid flat on the loading tray in a single layer with the paper side downwards on the tray surface to enable air removal and steam penetration.
Sterilisation cycle parameters
Follow the manufacturer’s instructions for steriliser use, for example only using distilled water. Each steriliser is designed to achieve specific sterilisation cycle parameters (time/temperature/pressure) that should not be altered without the manufacturer’s agreement.
Processing time
The total processing time for a load includes ‘penetration time’ plus ‘holding time’. The holding time is the time the whole load must be held at the sterilising temperature
The holding time includes a safety factor. Penetration time is the time taken for all parts of the load (inside the packaging) to reach the required sterilising temperature. All times and temperatures are based on the assumption that the items within the chamber are completely clean.
Penetration time
Penetration time is determined against the most difficult to sterilise package and the most difficult to sterilise load that the business intends to sterilise. Determining penetration time should be conducted by a service technician or suitably qualified person. Details of this process will need to be documented.
Holding time
The holding time is the time a load must be held at the sterilising temperature. The table below indicates required holding times according to temperature and pressure. All times and temperatures are based on the assumption that items being sterilised are completely clean.
Monitoring the sterilisation cycle
To ensure sterility, you should comply with performance testing and cycle monitoring as per AS/NZS 4815:2006. The selected cycle parameters, that is temperature, steam pressure and time, must be monitored and evidence provided that they have been met. There are three methods for monitoring the sterilisation cycle.
mechanical/physical indicators, that is, time and temperature monitoring, either manually or by automatic printout or computerised data logger
chemical indicators
biological/enzymatic indicators.
Mechanical/physical monitoring
All sterilisers should produce evidence that the selected sterilisation cycle parameters have been met. This may be via a process data logger or printer. Cycle parameters must be checked at the end of each cycle to ensure all parameters have been met. Results of the cycle (pass/fail) must be entered into the steriliser log.
If a process recorder printer or data logger is not working (for example, awaiting repairs to a faulty data logger or printer), then every sterilising cycle should be monitored every 10 seconds and the time, pressure and temperature of every cycle recorded. Existing sterilisers without process recorder/printers are obsolete and should be upgraded or replaced to ensure automatic parameter (time/temperature/pressure) monitoring and a permanent cycle record.
Chemical indicators
Chemical indicators are used in addition to mechanical/physical monitoring as part of the routine process for monitoring the sterilisation cycle. They are designed to monitor one or more sterilisation process parameters for the purpose of detecting equipment malfunction or sterilisation process failure.
Chemical indicators are divided into six classes, and various indicators are available (see Table 20: Classes of chemical indicators and their use below). The higher the class, the more information and specificity of the chemical indicator.
Chemical indictors are not to be used as a substitute for a permanent record of the sterilisation process (as per mechanical/physical monitoring). The exposed indicator may alter with time (for example, it may fade) and is not reliable for record-keeping. The result of the chemical indicator should be recorded into the steriliser log.
The manufacturer’s instructions should be followed when using chemical indicators. You should talk to the manufacturer (of both steriliser and indicator) about the best indicator to use, taking into account the types of item being sterilised, the type of packaging and the type of steriliser being used.
Chemical indicators should be used according to their classification, and a chemical indicator failure should be investigated to establish the cause of the failure of the sterilisation cycle before continuing to use the steriliser. Items from a sterilisation cycle with a failed chemical indicator should be re-cleaned and re-packaged before being re-sterilised.
Biological/enzymatic indicators
This type of indicator monitors the microbial killing power of the sterilisation process. Biological/enzymatic indicators may include bacterial spores, bacterial spores coated with an enzyme preparation, or enzymes extracted from bacterial spores. For steam sterilisation, the preferred test organism is Geobacillus stearothermophilus.
Biological/enzymatic indicators should be used:
after installation of a steriliser
after major repairs
as part of a validation procedure
to investigate cycle failures.
Biological indicators require incubation (to look for growth), whereas enzymatic indicators do not require incubation (the indicator will change colour with the drop of a solution after the cycle is completed).
Failures (that is, when growth is detected) should be investigated before continued use of the steriliser. Items from a sterilisation cycle process with a failed biological/enzymatic indicator must be completely reprocessed (that is, re-cleaned, re-packaged and re-sterilised).
Incubation of biological/enzymatic indicators should be conducted according to the manufacturer’s instructions (incubation kits are available from manufacturers). An indicator not exposed to the sterilisation process should also be incubated as a control for the exposed biological/enzymatic indicator. A permanent record of these results should be kept on file.
Unloading the steriliser
Drying cycle
Once drying stage of the cycle is complete, the load should be removed immediately from the chamber and visually inspected to ascertain that the load is dry, that the indicators used have changed to the required colour and that the seals are intact. Unpackaged items should not be directly handled, because this would render the item unsterile. All other parameters (time, temperature, pressure) should be checked, then recorded and signed as correct by the person removing the load. This is referred to as a parametric release.
Packaged items that are still damp at the end of the drying stage should not be considered sterile and should be fully reprocessed. Check both cycle parameters and the method of chamber loading to ascertain the cause of cycle failure. The number of items per load should be limited to allow the sterilising cycle to work effectively.
Items should be placed in an area where disturbance is minimal, to cool down. Forced cooling is not permitted because it will compromise the integrity of the item and its packaging. Items should not be placed directly onto solid surfaces during this cooling phase, because condensation will result from vapour still inside the package. Wet packaging, dropped items or non-intact seals mean the item cannot be considered sterile and should be fully reprocessed.
Without a drying cycle
Items processed without a drying cycle will be non-wrapped. Removal of these items will depend on whether the item is intended for immediate use or for storage and later use. Items for immediate use as sterile items should be removed using sterile gloves. Items for storage should be dried with a single-use lint-free cloth before being stored. It should be noted that unpackaged, stored items should not be used as sterile items and should be reprocessed prior to use if required to be sterile for use. Parameters (time, temperature, pressure) should be checked, then recorded and signed as correct by the person removing the load.
Storage of reprocessed items
All items must be stored in a manner that maintains their level of reprocessing. Sterilised packaged items should be stored in a way that will prevent contamination and damage to packaging. Storage may be in cupboards with close-fitting doors and smooth washable surfaces, or in washable plastic containers with close-fitting lids. Cupboards and containers should be moisture, dust, insect and vermin free, and used only for sterile items. Cupboards should be cleaned and dried weekly, and the cleaning process should not compromise sterility of the item.
Instruments must not be stored in disinfectants or under ultraviolet lamps before or after any form of reprocessing.
Ultraviolet cabinets are not suitable storage places. The ultraviolet rays act only on surfaces that they contact, and they damage packaging compromising sterility. Cardboard boxes are not suitable containers for storage of sterile items because they are porous, cannot be cleaned and may harbour harmful microorganisms. Items purchased sterile from commercial sources require similar storage conditions to those items sterilised in-house.
The shelf life of sterile stock is event-related. Influential factors on shelf life of sterile stock include the shelf life of the type of packaging material used (as per manufacturer’s recommendation), the type of storage and handling conditions (that is, the likelihood of product material deterioration and package design).
Ensure the oldest stock is used first. A sterile stock rotation system (for example place most recently sterilised items at the back of the storage container and only use stock from the front) should be implemented.
Factors that compromise sterile stock include incorrect cleaning procedures in storage areas, the presence of moisture and condensation, climatic extremes (that is temperature and humidity), excessive exposure to sunlight or other sources of ultraviolet light, vermin or insects, inappropriate packaging materials, incomplete sealing of packaging, the presence of sharp objects or rough handling causing damage, and incorrect handling during transportation.
Sterile stock should not be stored close to water sources (for example near sinks and hand basins) as water splashes onto sterile stock will render it ‘unsterile’. Excessive or rough handling and the use of rubber bands or other items that may damage packaging should not be used as these too will render stock unsterile.
Monitoring, validation and maintenance of sterilisers
Performance monitoring of sterilisers
Sterilisers require commissioning on installation before being used. Commissioning involves testing the steriliser cycle parameters for performance on-site. Performance testing or validation
p. 82) of the sterilising cycle parameters should be undertaken on installation, after routine servicing, after major repairs and when validating steriliser loads and packaging materials. Routine calibration testing should be performed at least every six months.
Monitoring of the sterilising process includes the cycle parameters, chemical and/or biological indicators results, load contents and number, date and time as previously discussed
Sterilisers may require leak, steam penetration and air removal tests between validations (for example a Bowie-Dick-type test). These should be conducted in accordance with the manufacturer’s recommendations.
Maintenance of sterilisers
Routine daily/weekly/monthly/quarterly scheduled maintenance as per the manufacturer’s recommendations must be performed as appropriate by trained staff and service personnel.
Loading trays should be cleaned daily and the steriliser cleaned when cool enough to permit the chosen cleaning agent to work efficiently and to prevent occupational health and safety hazards. The chamber drain should be kept clear and the recording device should function correctly. All gauges should be accurate, and the door gasket should be intact.
Validation of steriliser loads
Validation is required on commissioning (installation) prior to use and according to the manufacturer’s standards for performance. Validation is performed to evaluate the reliability of the sterilisation process and must be documented. It includes identification of the steriliser, the process parameters (time, temperature, pressure), steriliser chamber characteristics (such as hot and/or cold spots), the types of item(s) being routinely sterilised, and details of the cleaning and packaging processes used with the items being sterilised.
Three successful, consecutive and identical loads are required for a demonstrated validated cycle, although routine monitoring of the steriliser cycle is still required. Validation should be repeated if changes occur in the type of packaging used, major servicing of the steriliser is performed, the package contents are substantially changed, or the routine load or cycle parameters are changed.
Records
Results of all commissioning, validation and monitoring (daily and for each load) must be documented and maintained for a minimum period of 12 months. This also applies to other equipment that requires regular testing to confirm correct functioning and maintenance (for example ultrasound cleaner, heat sealing unit).





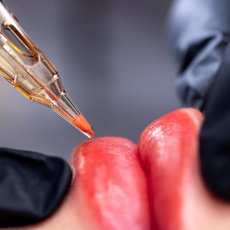


 Vectora Design
Vectora Design